Research - International Journal of Medical Research & Health Sciences ( 2023) Volume 12, Issue 7
A Case Study on the Effect of Physiotherapy on Joint Health and Functional Independence in a Person with Hemophilia who Underwent Upper Limb Fasciotomy
Sandeep Kumar1, Smati Sambyal1 and Akanksha Nagar2*2MPT (Neurology), University College of Physiotherapy, India
Akanksha Nagar, MPT (Neurology), University College of Physiotherapy, India, Email: akankshanaggar7@gmail.com
Received: 15-Jul-2023, Manuscript No. ijmrhs-23-106453; Editor assigned: 18-Jul-2023, Pre QC No. ijmrhs-23-106453(PQ); Reviewed: 22-Jul-2023, QC No. ijmrhs-23-106453(Q); Revised: 24-Jul-2023, Manuscript No. ijmrhs-23-106453(R); Published: 31-Jul-2023
Abstract
Background and Purpose: Persons with acquired or congenital hemophilia are at risk of developing acute compartment syndrome, which can complicate rehabilitation therapy. However, there is a lack of published literature on the role of physiotherapy in post-fasciotomy hemophilia cases. The study aims to investigate the impact of physiotherapy on post-operative upper limb fasciotomy in improving joint health, functional ability, range of motion and decreasing pain in person with hemophilia. Case Description: The case involves a 22 years old male subject with hemophilia A, diagnosed in 2004 with a factor assay of 1.2%. The subject presented with a history of left forearm pain after an intramuscular hematoma in the left forearm, leading to compartment syndrome and mild Volkmann ischemic contracture. The subject also experienced difficulty in gripping with the left hand and pain. Hemophilia Joint Health Score (HJHS), Functional Independence Score in Hemophilia (FISH), and score of Numeric Pain Rating Scale and Range of Motion were used as outcome measures. The physiotherapeutic interventions were given for 40 minutes for 4 weeks with five therapy sessions per week. Results: The findings of this study demonstrated a significant improvement in the outcome parameters with a decrease in HJHS score (8.8%), increase in score of FISH (15.6%), decrease in NPRS score (40%) and improved range of motion of wrist joint. Conclusion: In conclusion, this case study suggests that basic physiotherapy interventions lead to increased range of motion, improved joint health and decreased pain in post-operative cases of fasciotomy presenting as intramuscular hematoma with compartment syndrome in persons with hemophilia. These improvements contribute to enhanced functional independence.
Keywords
Compartment syndrome, Hemophilia, Post-operative fasciotomy, Physiotherapy, HJHS, FISH
Introduction
Hemophilia A and B are rare bleeding disorders caused by mutations in the factor VIII (FVIII) and factor IX (FIX) genes [1]. They are X chromosome-linked and have varying degrees of severity. Hemophilia A has a prevalence of 1 in 5000 male live births, while hemophilia B has a prevalence of 1 in 30,000 [1,2]. Acquired Hemophilia A (AHA) mainly affects the elderly and is often idiopathic. Hemophilia cases are under-diagnosed and under-registered, particularly in developing countries like India [3].
Persons with hemophilia are prone to spontaneous or traumatic bleeding, making them susceptible to Acute Compartment Syndrome (ACS). ACS is a condition characterized by increased pressure within a confined compartment, leading to tissue ischemia and potential limb loss, if left untreated. Bleeding in persons with hemophilia can occur in various locations, with subcutaneous bleeding being the most common in AHA. Approximately 70% of patients with bleeding episodes require hemostatic treatment [4]. Hemophilia primarily manifests with joint-related signs and symptoms, including chronic pain, muscle atrophy, limited range of motion, and deformity. While muscle bleeds accompanied by inflammation and contractures areless frequent, they can still occur. In managing hemophilia, physical therapy plays a critical role in several areas, including preventing new bleeds, restoring functionality, improving quality of life, and minimizing complications [4,5].
The POLICE method, which stands for Protection, Optimal load, Ice, Compression, and Elevation, is a recommended approach for initial management. It involves protecting the affected joints from further injury, using optimal loads during activities to avoid excessive stress on the joints, applying ice to reduce inflammation, utilizing compression techniques to control bleeding and swelling, and elevating the affected limb to minimize swelling [6]. Progressive muscle strengthening exercises are an integral part of physical therapy for individuals with hemophilia. These exercises aim to improve muscle strength, joint stability, and overall functional capacity. By gradually increasing the intensity and complexity of the exercises, individuals can enhance their muscular support around the joints and reduce the risk of bleeds [7-9]. Although there are some comprehensive healthcare centres providing treatment to People with Hemophilia (PWH), including surgical treatments, they remain inadequate, and their functioning is constrained by the cost of anti-hemophilic factors thus affecting the quality of life in haemophiliacs. Only a few case reports have focused on compartment syndrome in the realm of hemophilia A in the adult population [10,11]. Early recognition and treatment of an acute compartment syndrome is of extreme importance since in short term necrotic muscles can lead to rhabdomyolysis and renal failure and even a “crush syndrome” in which myoglobinuria, hyperkalemia and acidosis can lead to renal failure, shock and cardiac arrhythmias. Longterm the necrotic muscle tissue will lead to a Volkmann’s contracture [12]. About 1% to 10% of the patients with an acute compartment syndrome develop Volkmanns contracture [13]. There is a lack of published studies on physiotherapy postoperative management of compartment syndrome associated with hemophilia A and there was inadequate data describing this entity on the upper extremities. Therefore, this case study consisted of person with traumatic compartment syndrome of forearm due to hemophilia A, which was treated surgically with a long and complicated postoperative course.
Case Presentation
This case study focused on a 22 years old male subject presented to the physiotherapy OPD with a diagnosis of Hemophilia A in 2004, having factor assay of 1.2%. The subject had a history of a fall, resulting in swelling on his left forearm and hand due to intramuscular bleeding. Initially, fresh frozen plasma was administered for management, but the symptoms worsened. As a result, the subject underwent surgical procedure, which involved fasciotomy, hematoma evacuation with the administration of factor VIII. Intraoperative findings revealed an “s” shaped incision on the volar aspect of the left forearm, along with a large 8 cm × 6 cm intramuscular hematoma within the flexor digitorum profundus. After the surgery, a thorough examination revealed concerning findings regarding the flexor digitorum profundus and pronator quadratus muscles. These muscles were found to be in an unhealthy state, exhibiting necrotic tissue and lacking the ability to contract effectively.
Following the fasciotomy, necrotic muscle tissue was visible on the flexor aspect of the forearm. The fasciotomy wound was extended distally up to the wrist joint and 4 cm distal to the elbow joint. The distal part of the flexor digitorum profundus, which was necrosed and non-contractile, was excised while preserving the tendon. Some necrosed fibers of the flexor digitorum superficialis were also removed. Hydrobeta wash was administered, and hemostasis was achieved. Throughout the hospital stay, the subject remained hemodynamically stable, and the wound showed signs of healing. On day 1 after surgery, the subject's wound remained healthy, but the flexor muscle exhibited mild dusky appearance and contracture in flexion. On day 4, redebridement was performed. By day 5, the subject's wound was healthy, and a hematology consultation was conducted regarding the administration of factor VIII. On day 6, the subject remained hemodynamically stable, and the wound was healing.
Radiological investigations using ultrasonography of the left upper limb Doppler, revealed a large, relatively welldefined heterogenous hypoechoic lesion on the medial and ventral aspects of the left forearm. Associated subcutaneous tissue edema and a 20 cm × 3.5 cm fluid fat lesion showed no intact vascularity. The radial artery exhibited attenuation in caliber at the level of the mid-forearm in relation to the hematoma, but normal caliber was observed at the wrist. No obvious filling defect was observed
After a week of post-operative care and monitoring, the subject was discharged from the hospital. Following 10 days of discharge, the subject presented to the physiotherapy OPD. with a chief complaint of difficulty in gripping with his left hand, accompanied by forearm pain. These symptoms had developed a week after the removal of an intramuscular hematoma through fasciotomy and debridement in the left forearm. The subject reported limitations in holding fine objects and performing wrist extension. The pain was described as a dull ache, which was generally relieved with medications. The subject had also a known history of HCV infection and a family history of haemophilia, as his maternal uncle was diagnosed with the same condition
On examination, the subject's wound appeared healthy with no signs of swelling. A pre-assessment was conducted, which included the administration of outcome measures to evaluate the subject's condition. The Hemophilia Joint Health Score (HJHS) was used to assess joint health, with a recorded score of 22 out of 124 The Functional Independence Scale in Hemophilia (FISH) was utilized to evaluate the subject's functional independence, with a recorded score of 18 out of 32. The subject's wrist joint passive Range of Motion (ROM), measured with goniometer revealed 8° of passive wrist flexion with fingers flexed and passive wrist extension recorded as 20° with flexion of fingers while no active wrist extension was observed. The wrist ulnar and radial deviation was found to be 22° and 10° respectively. Furthermore, the subject exhibited a loss of sensation of pain and light touch over the hypothenar eminence and the volar aspect of the fingers. This was assessed by lightly touching or stroking with tissue for light touch sensation and using the sharp end of a reshaped paper clip for pain sensation, respectively.
Interventions
During the physiotherapeutic interventions, the subject visited the physiotherapy OPD three to four times a week after the administration of factor VIII according to the dosage calculated by given formula; [Body Weight (BW) (kg) × desired FVIII increase (%)]/2 [14]. The duration of each interventional session was approximately 40 minutes for 4 weeks with five therapy sessions per week. During the first two weeks of the physiotherapy intervention, the focus was on active exercises within a pain-free range of affected joint. For the wrist joint, flexion and extension exercises were performed for 8 repetitions once a day. Additionally, radial and ulnar deviations were included in the exercise routine, also performed for 8 repetitions with one set. The repetitions and sets were planned according to Guidelines for the management of Hemophilia [15]. The goal of these exercises was to improve the range of motion and strength of the wrist joint.
Further, the subject performed flexion, extension, supination, and pronation exercises of elbow joint, with assistance as needed. Each exercise was repeated 12 times of one set to enhance joint flexibility and muscle strength in the elbow region. For the shoulder joint, the subject actively performed exercises involving flexion, extension, abduction, adduction, external rotation, and internal rotation for 12 repetitions, one set.
After the completion of initial phase, the following third and fourth weeks of the intervention program, the exercises involved were passive exercises with distraction of wrist joint and resisted exercises of elbow and shoulder joint. The purpose of these exercises was to further improve joint mobility. The subject's wrist joint underwent exercises encompassing flexion, extension, radial deviation, and ulnar deviation. These passive exercises were performed in the full range of motion for the wrist joint and repeated 12 times once a day. Further, the subject actively engaged in an isometric wrist extension exercise, by applying resistance against a cushioned surface for 8 seconds per repetition, completing 5 repetitions, one set. This isometric contraction promotes strength and stability in the wrist joint. In addition to the isometric wrist extension, the subject also performed a wrist exercises using a ball by gripping it firmly and squeezing it for a 12 number of repetitions of two sets. To further enhance hand grip, the subject was also engaged in flat peg board exercises by placing and removing pegs in different patterns or designs. These exercises on the flat peg board helped improve finger strength, hand-eye coordination and gross grip strength. As for the elbow joint, resisted exercises were incorporated. The subject performed resisted flexion, extension, supination, and pronation exercises. By applying resistance during these movements, the muscles surrounding the elbow joint were further engaged, enhancing their strength and stability. Each exercise was repeated 12 times with one set to maximize the benefits.
In the case of the shoulder joint, resisted exercises involving flexion, extension, abduction, adduction, external rotation, and internal rotation were performed. These exercises targeted the muscles responsible for the movement and stability of the shoulder joint. By applying resistance during these movements, the subject worked on improving the strength and control of the shoulder joint. Each exercise was performed 12 times to ensure an adequate training stimulus.
In the physiotherapeutic interventions of 4 weeks duration, the repetitions of exercises were according to the tolerance level of subject after the administration of factor VIII.
Results
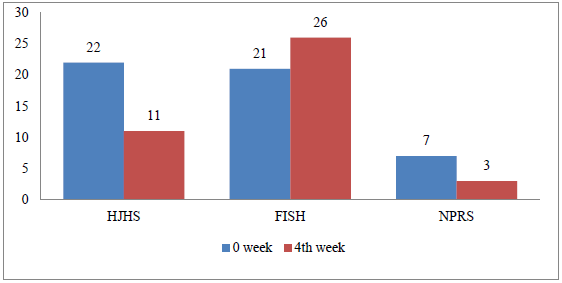
The re-evaluation was conducted to assess the outcomes of the intervention after 4 weeks of physiotherapeutic interventions. The baseline scores for HJHS and FISH were 22 and 21, respectively. Post-intervention results showed a significant improvement in both scores, with score of 11 for HJHS (8.8% decrease) indicating improved joint health and 26 for FISH (15.6% increase) indicating improvement in functional independence. The pain was reduced from the score of 7 on Numerical Pain Rating Scale to 3 (40%). These findings indicated a notable enhancement in the subject's joint health and functional independence with reduction of pain following the physiotherapy intervention as described in Table 1 and represented in Figure 1 respectively.
| Outcome measure
|
Pre interventional score
|
Post interventional score
|
|---|---|---|
| (0 week)
|
(4th week)
|
|
| HJHS
|
22
|
11
|
| FISH
|
21
|
26
|
| NPRS
|
7
|
3
|
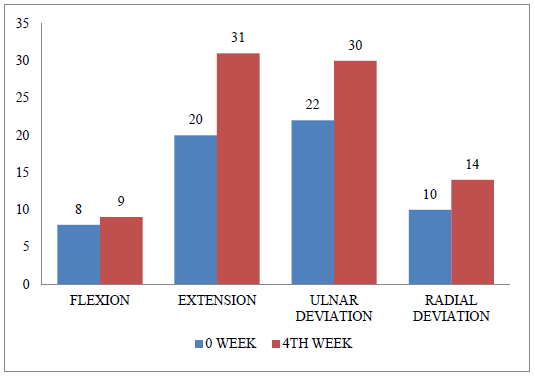
The Range of Motion (ROM) of the wrist joint was assessed using goniometer before and after the intervention. At the pre-intervention stage (0 week), the measurements indicated that the subject had a wrist flexion (passive) of 8°, which increased to 9° by the fourth week. Similarly, the wrist extension (passive) improved from 20° initially to 31° after the intervention. The patient's ability for ulnar deviation of the wrist also showed positive progress, increasing from 22° to 30° over the four-week period. Additionally, the range of motion for radial deviation of the wrist improved from 10° at the beginning to 14° after the intervention. These findings were described in Table 2 and displayed in Figure 2 respectively.
| Range of Motion of wrist joint
|
Pre interventional range
|
Post interventional range
|
|---|---|---|
| (0 week)
|
(4th week)
|
|
| Wrist flexion (Passive)
|
8°
|
9°
|
| Wrist extension (Passive)
|
20°
|
31°
|
| Wrist ulnar deviation
|
22°
|
30°
|
| Wrist radial deviation
|
10°
|
14°
|
Discussion
This case study demonstrated improvement in the subject's ability to grip objects and an increased range of motion. The subject reported being able to hold gross objects more firmly, suggesting enhanced hand strength. Additionally, the achieved stability implies improved joint stability and control, leading to better functional outcomes. Moreover, the subject experienced improved wound healing, which could be attributed to the circulation-enhancing effects of the upper extremity exercises performed during the physiotherapy sessions.
Hemophilia often leads to joint stiffness and limited range of motion due to recurrent bleeding episodes and subsequent joint damage. Exercises that focus on joint mobilization help to improve joint flexibility and increase the range of motion. By engaging in these exercises regularly over the 4-week period, the subject may have experienced reduced joint inflammation, increased range of motion of wrist joint and improved overall joint function. These factors would contribute to a decrease in the HJHS score, indicating enhanced joint health. This is in accordance with the study done by Maria Helena et al., as they also concluded that rehabilitation program positively influence the joint heath status and quality of life in 24 persons with haemophilia [16].
The FISH is a measure that evaluates functional independence in individuals with hemophilia. The physiotherapy intervention likely focused on enhancing the subject's ability to perform daily activities and tasks independently. The improvements in physical abilities and functional independence would result in an increase in the FISH score which is also documented by Ripudaman Singh et al., in which they reported improvement in the scores of HJHS and FISH with the administration of physiotherapeutic interventions in 18 patients [17].
Following a fasciotomy, scar tissue formation is common. Physiotherapy interventions, including scar tissue massage and mobilization techniques, for the duration of 4 weeks, prevent excessive scar tissue adhesion, improve tissue flexibility, and reduce pain associated with scar tissue formation. These techniques promote optimal healing and minimize pain and discomfort. R. Beyer conducted the study which documented the physiotherapeutic interventions improve scar formation [18].
In this case, although the subject had not achieved normal Range of Motion (ROM), they did demonstrate significant improvement in their functional range of motion of wrist joint [19]. Several factors can be attributed to the successful outcomes observed. Firstly, the prompt diagnosis of the subject's condition enabled early intervention,which is crucial for optimizing treatment outcomes. Secondly, the subject's age, fitness level, and overall health (without any co-morbidities) likely played a role in their positive response to the physiotherapeutic management. These factors may have facilitated a more favourable healing process and enhanced functional recovery.
It is important to note that this case description presents a single subject's experience, and further research with larger sample sizes and controlled study designs would be necessary to generalize the findings. Additionally, the specific physiotherapy interventions utilized in this case may not be universally applicable and should be tailored to individual subjects' needs and condition severity. Nonetheless, the results of this study indicate the potential benefits of physiotherapy in improving joint health, functional independence, range of motion of wrist joint and reducing pain in subjects with similar conditions.
The present study has certain limitations that should be acknowledged. Firstly, the study is based on the experience of only one individual, which limits its external validity and generalization to a larger population. Further research involving larger sample sizes would be necessary to validate the findings and draw more robust conclusions.
Furthermore, it is important to note that this study was conducted in a smaller geographical area and represents the first of its kind in this context. The limited availability of published literature specific to this region meant that the physiotherapy approach utilized in this study was based on basic therapeutic principles. While this approach may have been effective in this case, it is essential to acknowledge the need for further research and exploration of more advanced and specialized techniques for optimal subject outcomes. Additionally, future studies could focus on incorporating a wider range of electrotherapy modalities to enhance the postoperative management of compartment syndrome associated with hemophilia A.
Conclusion
In conclusion, this case study highlights the positive impact of basic physiotherapy interventions on a postoperative case of fasciotomy presenting as intramuscular hematoma with compartment syndrome. The findings indicate that through the implementation of these interventions, the subject experienced increased range of motion, improved muscular strength, and enhanced grip stability, which contributed to their functional independence. However, considering the limitations mentioned earlier, further research is warranted to validate these findings and explore more advanced physiotherapy techniques for similar cases
Overall, this study contributes to the existing knowledge by demonstrating the potential benefits of physiotherapy in the management of postoperative complications associated with intramuscular hematoma and compartment syndrome. Further research in larger populations and diverse settings is necessary to enhance the understanding and optimize the physiotherapeutic approaches for such cases
Declarations
Conflicts of Interest
The authors and planners have disclosed no potential conflicts of interest, financial or otherwise.
Source of Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
References
- Peyvandi, F., et al. "Genetic diagnosis of haemophilia and other inherited bleeding disorders." Haemophilia, Vol. 12, 2006, pp. 82-89.
Google Scholar Crossref - Franchini, Massimo. "The modern treatment of haemophilia: a narrative review." Blood Transfusion, Vol. 11, No. 2, 2013, p. 178.
Google Scholar Crossref - Collins, Peter, et al. "Consensus recommendations for the diagnosis and treatment of acquired hemophilia A." BMC research notes, Vol. 3, No. 1, 2010, pp. 1-8.
Google Scholar Crossref - Dolan, Gerry, et al. "Principles of care for acquired hemophilia." European journal of haematology, Vol. 106, No. 6, 2021, pp. 762-73.
Google Scholar Crossref - Van Vulpen, L. F. D., K. Holstein, and C. Martinoli. "Joint disease in haemophilia: pathophysiology, pain and imaging." Haemophilia, Vol. 24, 2018, pp. 44-49.
Google Scholar Crossref - Tusell, J. M., et al. "Results of an orthopaedic survey in young patients with severe haemophilia in Spain." Haemophilia, Vol. 8, 2002, pp. 38-42.
Google Scholar Crossref - Srivastava, Alok, et al. "WFH guidelines for the management of hemophilia." Haemophilia, Vol. 26, 2020, pp. 1-158.
Google Scholar Crossref - McLaughlin, Paul, et al. "Physiotherapy interventions for pain management in haemophilia: a systematic review." Haemophilia, Vol. 26, No. 4, 2020, pp. 667-84.
Google Scholar Crossref - Pacheco-Serrano, Ana I., David Lucena-Anton, and José A. Moral-Muñoz. "Rehabilitación física en pacientes con artropatía hemofílica: revisión sistemática y metaanálisis sobre dolor." Revista Colombiana de Reumatología, Vol. 28, No. 2, 2021, pp. 124-33.
Google Scholar Crossref - Weng, Yi-Ming, and Cheng-Ting Hsiao. "Acquired hemophilia A associated with therapeutic cupping." The American journal of emergency medicine, Vol. 26, No. 8, 2008, p. 970.
Google Scholar Crossref - Ilyas, Asif M., et al. "Upper extremity compartment syndrome secondary to acquired factor VIII inhibitor: a case report." JBJS, Vol. 87, No. 7, 2005, pp. 1606-08.
Google Scholar Crossref - Heemskerk, V. H., et al. "The acute compartment syndrome of the arm." Nederlands tijdschrift voor geneeskunde, Vol. 148, No. 45, 2004, pp. 2235-40.
Google Scholar - Leversedge, Fraser J., et al. "Compartment syndrome of the upper extremity." The Journal of hand surgery, Vol. 36, No. 3, 2011, pp. 544-59.
Google Scholar Crossref - Henrard, Séverine, Niko Speybroeck, and Cedric Hermans. "Impact of being underweight or overweight on factor VIII dosing in hemophilia A patients." Haematologica, Vol. 98, No. 9, 2013, p. 1481.
Google Scholar Crossref - Srivastava, Alok, et al. "Guidelines for the management of hemophilia." Haemophilia, Vol. 19, No. 1, 2013, pp. 1-47.
Google Scholar Crossref - Meiklejohn, D. J., and H. G. Watson. "Acquired haemophilia in association with organ‐specific autoimmune disease." Haemophilia, Vol. 7, No. 5, 2001, pp. 523-25.
Google Scholar Crossref - Podolak-Dawidziak, Maria Helena, et al. "The Influence of Personalized 2-Year Physiotherapy on Musculoskeletal Health and Quality of Life in Severe Hemophilia Patients with Inhibitor-Interim Analysis after 1 Year of the Program." Blood, Vol. 136, 2020, p. 36.
Google Scholar Crossref - Singh, Ripudaman, et al. "Responsiveness to hemophilia joint health score and functional independence score in patients with hemophilia with intermittent factor support and physiotherapy." CHRISMED Journal of Health and Research, Vol. 8, No. 3, 2021, pp. 187-91.
Google Scholar Crossref - Palmer, Andrew K., et al. "Functional wrist motion: a biomechanical study." The Journal of hand surgery, Vol. 10, No. 1, 1985, pp. 39-46.
Google Scholar Crossref