Case Report - International Journal of Medical Research & Health Sciences ( 2025) Volume 14, Issue 7
A Fatal Combination: Miliary Tuberculosis and Acute Respiratory Distress Syndrome-A Case Report
A. Karim*, A. Kumar, A. K. Gupta, A. K. Gautam, P. Yadav and S. Bhattacharya SA. Karim, Department of Respiratory Medicine, Uttar Pradesh University of Medical Sciences, Saifai, Etawah, India, Email: drakbest@ymail.com
Received: 06-Oct-2024, Manuscript No. IJMRHS-24-149648; Editor assigned: 09-Oct-2024, Pre QC No. IJMRHS-24-149648 (PQ); Reviewed: 24-Oct-2024, QC No. IJMRHS-24-149648; Revised: 04-Jul-2025, Manuscript No. IJMRHS-24-149648 (R); Published: 11-Jul-2025
Abstract
A rare and fatal complication of miliary tuberculosis is Acute Respiratory Distress Syndrome (ARDS). We present a case of a 22-year-old male with an eight-month history of weight and appetite loss, and rapidly worsening dyspnea over 15 days, leading to ICU admission. Chest X-ray and CT revealed bilateral miliary opacities. Blood tests showed hyponatremia and leukocytosis. The patient received non-invasive ventilation, intravenous corticosteroids, and anti-tubercular therapy based on clinical and radiological findings. After one month in the ICU, he showed rapid improvement following treatment.
Keywords
Dexamethasone, Antitubercular therapy, Hyponatremia, Acute respiratory distress syndrome, Miliary tuberculosis
Introduction
Miliary Tuberculosis (TB) occurs due to widespread lymphohematogenous spread of Mycobacterium tuberculosis, resulting in a distinctive presentation. Miliary TB is characterized by the presence of tiny nodules resembling millet seeds in both appearance and size [1].
Clinically, miliary TB presents with non-specific symptoms such as chronic fever, weight loss, and reduced appetite. Pulmonary involvement often leads to symptoms like a productive cough and shortness of breath. Due to the nonspecific nature of these symptoms, diagnosis is frequently delayed. In rare cases, miliary TB can present as Acute Respiratory Distress Syndrome (ARDS), particularly in patients with extensive lung involvement [2].
Chest radiographs typically show a "miliary" pattern, marked by numerous small nodular shadows spread across the lungs. In countries with high TB prevalence, such as India, maintaining a high level of suspicion for miliary TB in patients with non-specific symptoms is crucial to ensure timely diagnosis and treatment.
Case Presentation
A 22-year-old male patient presented to the Emergency Department with complaints of gradually progressive breathlessness for three months, which had increased significantly over the last 10 days, dry cough, fever, vomiting, and loss of appetite.
The patient also reported chronic complaints of left-sided chest pain and weight loss for eight months. Given his worsening oxygenation situation, the patient was admitted to the intensive care unit and started on non-invasive ventilation with oxygen support.
The patient had no history of comorbid conditions apart from chronic alcohol consumption for four years. On general examination, his findings were as follows: Pulse rate: 128 beats/minute; Respiratory rate: 28 breaths/minute; Blood pressure: 90/50 mm Hg; and Oxygen saturation (SpO2 %): 88% on oxygen. Pallor was present, while icterus was absent, and chest auscultation revealed the presence of bilateral crepitations.
Laboratory investigation revealed WBC 4300 cell/mm3 lymphocytes 26%, and Neutrophil 75.6% monocytes 2.5%, hemoglobin of 9.3 g/dl, and platelet count of 1.95 lac cell/mm3.
His liver enzymes, aspartate transaminase 61 IU/L, alanine transaminase 51 IU/L, and alkaline phosphatase 501 IU/L. Gamma glutamyl transpeptidase was 160 IU/L, total bilirubin 0.9 mg/dl, and albumin 2.3 g/l. Random glucose was 110 mg/dl, erythrocyte sedimentation rate 30 mm/h, and C-reactive protein 203 mg/L.
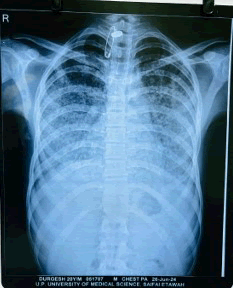
His blood chemistry and coagulation profile were within normal limits. Arterial blood gases, on oxygen by face mask were pH 7.40, partial pressure of arterial carbon dioxide (PaCO2) 37.5 mmHg, partial pressure of arterial oxygen (PaO2) 68.5 mmHg, and bicarbonate concentration 21 mmol/L, Chest X-ray pa view showing bilateral symmetrical miliary opacities (Figures 1-3).
Figure 1 Chest X-ray showing bilateral symmetrical miliary opacities
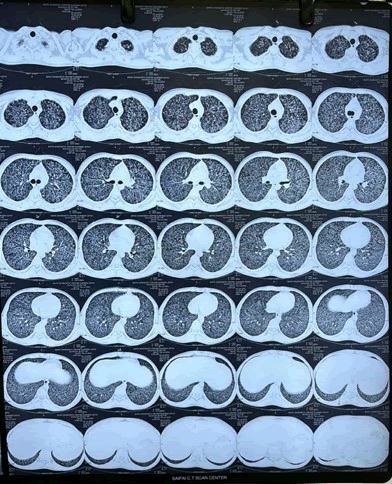
Figure 2 HRCT thorax showing diffuse bilateral nodular opacities with bilateral ground glass opacities
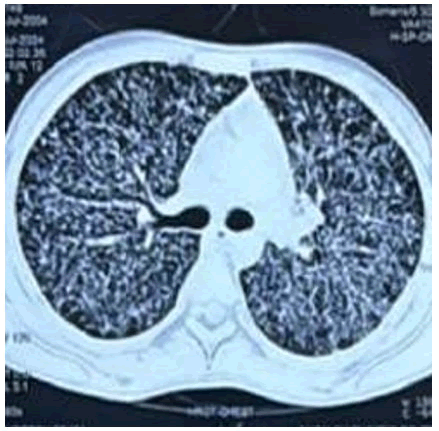
Figure 3 HRCT thorax showing diffuse bilateral nodular opacities.
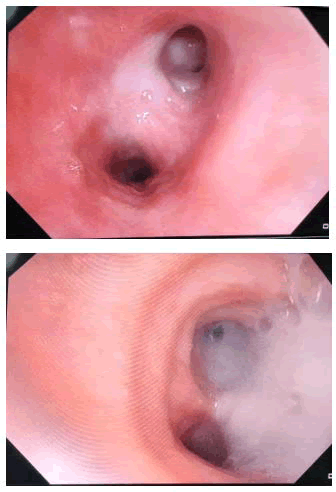
A flexible fiber optic bronchoscopy was done, which showed the presence of thick mucopurulent secretions present in the Right bronchial tree. No visible endobronchial mass or anatomical abnormality was observed bronchoalveolar lavage fluid for malignant cells Negative (Figure 4).
Bronchoalveolar Lavage (BAL) for AFB/MTB/RIF (GeneXpert)=MTB not detected
Flexible Bronchoscopy (thick mucoprulent).
Ultrasonography of the abdomen=Mild hepatosplenomegaly
Tuberculin Skin Test (TST)=Positive
Fundoscopy=Choroidal tubercles present all over fundus.
Figure 4 Flexible bronchoscopy (thick mucoprulent)
Laboratory studies showed anemia, elevated ESR. Arterial blood gas analysis revealed severe hypoxemia, confirming the diagnosis of ARDS. A proper history ruled out other etiologies such as occupational lung diseases and hypersensitivity pneumonitis.
A high-resolution chest CT scan confirmed the diagnosis, showing multiple miliary nodules scattered throughout the lungs. A flexible fiber optic bronchoscopy was done, which showed the presence of thick mucopurulent secretions present in the right bronchial tree. No visible endobronchial mass or anatomical abnormality was observed bronchoalveolar lavage fluid for malignant cells Negative
Based on the clinical presentation, radiological findings, positive TB tests, and fundoscopy findings, a diagnosis of miliary tuberculosis with secondary ARDS was made
After initiating Non-Invasive Ventilation (NIV) support and Anti-Tubercular Therapy (ATT), the patient's oxygenation and blood parameters began to improve. He was gradually weaned off oxygen support and transferred to the general ward.
The patient was discharged after 21 days on ATT, with a standard four-drug regimen consisting of Isoniazid (H), Rifampicin (R), Pyrazinamide (Z), and Ethambutol (E), to be continued for six months.
Discussion
Miliary Tuberculosis (TB) refers to the lymphohematogenous spread of TB bacilli throughout the body from the primary site of infection. If left untreated, it almost always leads to death [3]. In countries with a low-to-moderate incidence of TB, the mortality rate for treated miliary TB patients is around 14%. However, the risk of death increases when complications such as ARDS, multi-organ failure, and septic shock occur [4].
Early diagnosis and prompt treatment are crucial to improve patient outcomes. Common non-specific symptoms of miliary TB in adults include weight loss, loss of appetite, chills, and night sweats, along with pulmonary symptoms like cough with expectoration, breathlessness, and chest pain [5]. On physical examination, findings may include tachypnea, cyanosis, hepatosplenomegaly, and, in some cases, choroidal tubercles or ascites.
Although ARDS is a rare complication of miliary TB, affecting fewer than 8% of patients, it is associated with a high mortality rate of 40-80%, even with corticosteroids and mechanical ventilation. Delayed diagnosis or failure to diagnose often contributes significantly to the high mortality of miliary TB patients [6]. However, early initiation of Anti-Tubercular Therapy (ATT), careful use of corticosteroids, and access to critical care can significantly reduce mortality rates [7].
Conclusion
This case report describes a young male patient with miliary TB that progressed to ARDS. The patient showed significant improvement following aggressive treatment for hypoxia, along with early initiation of corticosteroids and Anti-Tubercular Therapy (ATT). Without timely medical intervention and critical care support, such as Non- Invasive Ventilation (NIV), his condition would likely have worsened rapidly. This case underscores the importance of early and aggressive intervention, particularly ATT, in patients with ARDS who present with radiological evidence of miliary TB.
References
- Sharma SK, Mohan A and Sharma A. Challenges in the diagnosis and treatment of miliary tuberculosis. Indian Journal of Medical Research. Vol.135, No.6, 2012, pp. 703-730.
[Google Scholar] [PubMed]
- Mohan A, Sharma SK and Pande JN. Acute respiratory distress syndrome (ARDS) in miliary tuberculosis: A twelve-year experience. The Indian Journal of Chest Diseases & Allied Sciences. Vol.38, No.3, 1996, pp. 157-162.
[Google Scholar] [PubMed]
- Sharma SK, et al. Miliary tuberculosis: New insights into an old disease. The Lancet Infectious Diseases. Vol.5, No.7, 2005, pp. 415-430.
[Crossref] [Google Scholar] [PubMed]
- Mert A, Arslan F and Kuyucu T. Miliary tuberculosis: Epidemiologicaland clinical analysis of large-case series from moderate to low tuberculosis endemic country. Medicine (Baltimore). Vol.96, No.5, 2017, pp. e5875.
[Crossref] [Google Scholar] [PubMed]
- Reichmann MT, et al. Tuberculosis and TNF-inhibitors: History of exposure should outweigh investigations. BMJ Case Reports. Vol.2014, 2014.
[Crossref] [Google Scholar] [PubMed]
- Singh K, et al. Miliary tuberculosis presenting with ARDS and shock: A case report and challenges in current management and diagnosis. Case Reports in Critical Care,. Vol.2017, pp. 9287021.
[Crossref] [Google Scholar] [PubMed]
- Aurangabadkar GM, et al. Miliary tuberculosis with acute respiratory distress syndrome: A deadly combination. Cureus. Vol.15, No.1, 2023, pp. 33944.
[Crossref] [Google Scholar] [PubMed]