Research - International Journal of Medical Research & Health Sciences ( 2022) Volume 11, Issue 1
Atypical Holt-Oram Syndrome Presenting with Renal Agenesis: A Case Report
Jyoti Jain1*, Saiprasath Janaarthanan1, Babita Bondge1, Shahryar Khan1, Madhura Joshi1 and Tanvi Banait22Department of Medicine, Jawaharlal Nehru Medical College, Sawangi, Wardha, Maharashtra, India
Jyoti Jain, Department of Medicine, Mahatma Gandhi Institute of Medical Sciences, Sevagram, Wardha, Maharashtra, India, Email: jyotijain@mgims.ac.in
Received: 12-Dec-2021, Manuscript No. ijmrhs-22-51586 (M); Accepted Date: Jan 21, 2022 ; Editor assigned: 14-Jan-2022, Pre QC No. ijmrhs-22-51586 (P); Reviewed: 20-Jan-2022, QC No. ijmrhs-22-51586 (Q); Revised: 22-Jan-2022, Manuscript No. ijmrhs-22-51586 (R); Published: 29-Jan-2022
Abstract
Holt-Oram syndrome is a rare congenital anomaly; however, it is the most common type of Heart-Hand syndromes. It is characterized by absent radial bone, an Atrial Septal Defect (ASD), most commonly an ostium secumdum type, and heart blocks. This patient was a 17-year male who was having a short right upper limb, absent right thumb, and a supernumerary digit since birth. Recently he had been having dyspnoea on exertion and palpitations and Echocardiography (ECHO) revealed an ostium secundum type of ASD and the patient was referred to our tertiary care centre for the closure of an ASD. On evaluation, his X-ray right arm was suggestive of the absent radial bone. Routine sonography of the abdomen was done to rule out other defects which surprisingly revealed an absent right kidney. His ASD was corrected using a 28 mm closure device under fluoroscopic guidance and the post-procedure course was uneventful. The patient was counseled about his deformity, sensitized with a single functioning kidney, advised on rehabilitation, and discharged. Here we describe a case of atypical Holt-Oram syndrome with a single functioning kidney.
Keywords
Absent of radius, Atrial Septal Defect (ASD), Deformities, Heart-Hand syndromes, Holt-Oram Syndrome
Introduction
Heart-Hand syndromes or cardiomyelic syndromes are a variety of disorders characterized by limb anomalies and cardiac, valvular, or septal defects which may also be associated with conduction blocks. A few other subtypes of these syndromes include Berk-Tabatzik syndrome, Patent ductus arteriosus-bicuspid aortic valve syndrome, Heart- Hand syndrome of Slovenian type. The prototype and most common type is the Holt-Oram syndrome, which is characterized by absent radial bone, ASD (most commonly an ostium secumdum type), and heart blocks.
Holt-Oram syndrome has an autosomal dominant pattern of inheritance, however, 85% of the affected people have sporadic mutations (TBX5 gene mutation in chromosome 12) with normal parents [1]. It is seen that the incidence is increased with consanguinity [2]. The affected patients have a limb anomaly from birth, normal intellectual development, and a cardiac septal defect which is usually asymptomatic until the fourth decade. Most patients have severe symptoms only during their fourth decade of life, which gives enough time to correct these defects. Here we describe a case of Holt-Oram syndrome with an atypical presentation in the form of kidney agenesis.
Case Report
A 17-year male patient with, a known case of ASD was referred to our hospital for ASD correction. His chief complaints on admission were dyspnoea on exertion and palpitations for 2 years. His dyspnoea was insidious in onset, intermittent in nature, associated with physical activity of NYHA Grade 2. The patient also had a history of intermittent palpitations which were not associated with the activity. There was no history of chest pain, fever, cough, giddiness, and loss of consciousness. The patient had a history of uneventful normal vaginal home delivery. His mother did not have any history of teratogenic drug intake, good nutrition including folic acid and iron supplement was present to the mother during her antenatal period. He attained his development milestones at a proper age. At the age of 5 years, he was diagnosed with ASD and advised for closure of ASD after a few years. There was no history of cyanosis, giddiness, recurrent chest infections, and multiple hospital admissions. His scholastic performance was normal for his age. There was no significant family history of cardiac illness or any congenital anomalies.
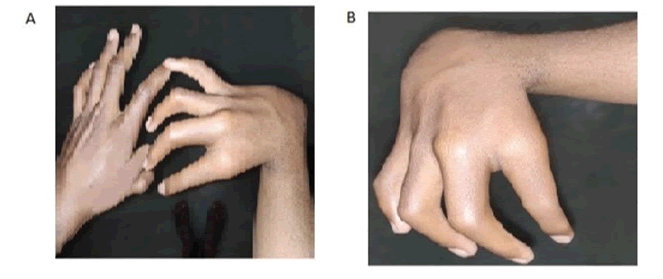
On general examination, he was conscious, oriented within normal mental functions. He was afebrile with a pulse was 120 bpm, blood pressure of 110/80 mm Hg, normal JVP, and normal height and weight for his age. Pallor, clubbing, cyanosis, pedal edema, icterus, and lymphadenopathy were absent. He has an absent thumb in the right hand, varus deformity of the right forearm, shortening of the right forearm with muscle agenesis, and polydactyly in the left hand (Figure 1A and Figure 1B). On cardiovascular examination, the apex beat was present in the left 5th intercostal space in the midclavicular line of heaving nature. Systolic thrill present in the left apical region. On auscultation, early to mid-systolic, a grade V murmur was present in the left second intercostal space at the sternal border. Loud P2 with wide fixed splits and opening snaps were present but no S3 and S4 were heard. The rest of the systemic examination was normal.
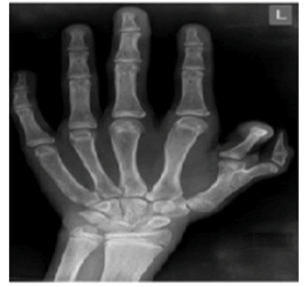
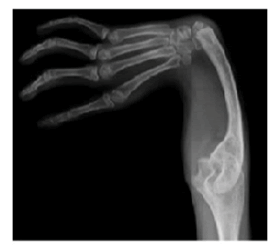
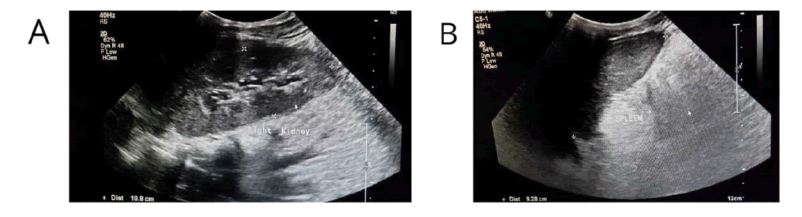
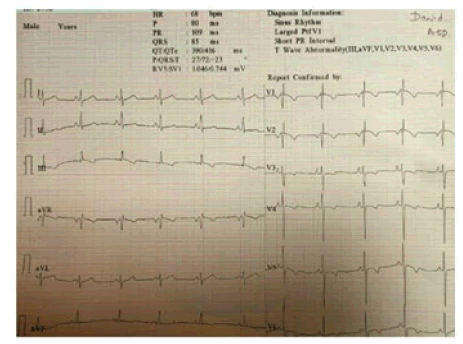
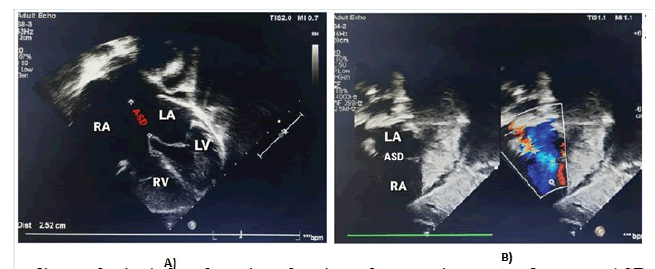
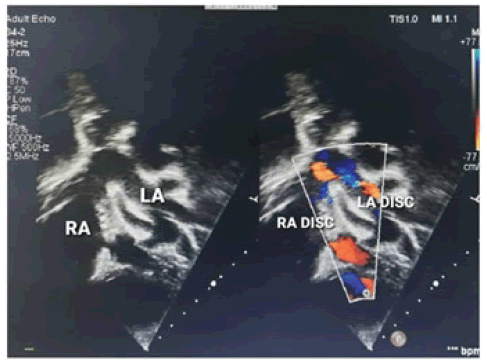
Haematological and biochemical tests including complete blood count, random plasma glucose, serum electrolytes, renal function test, and liver function, were within normal limits for age, but he had mild anaemia with haemoglobin of 10.7 gm. His left-hand X-ray revealed a supernumerary digit due to the presence of a bifid first metacarpal bone with an extra proximal phalanx (Figure 2). His X-ray right forearm revealed the absence of radius bone with an absent thumb and missing carpal bone (Figure 3). His ultrasound abdomen revealed the absence of the right kidney (Figure 4A and Figure 4B). The Electrocardiogram (ECG) showed biventricular hypertrophy, left atrial enlargement, incomplete RBBB with normal axis (78 degrees), and LVH strain pattern (Figure 5). Pre-procedure 2D ECHO revealed large secundum ASD along with significant right ventricular enlargement, pulmonary pressure of 35 mmHg systolic, and normal pulmonary venous drainage. Nearly 4 mm atrioventricular rim was deficient all other rims were adequate and no other structural abnormality was found (Figure 6A and Figure 6B).
Figure 5. A-A standard 12 lead ECG showing a heart rate of 68 bpm, sinus rhythm, normal axis (78 degrees), negative P wave in lead V1 (4 mm in amplitude and 80 ms wide), PR interval 0.12 sec, QRS duration 0.08sec, rSR’ pattern in lead V1 and V2, T wave inversion in III and all chest lead suggestive of left atrial enlargement, incomplete right bundle branch block strain pattern, biventricular hypertrophy and LVH strain pattern
ASD closure was done under ECHO and fluoroscopic guidance with a 28 mm ASD device with good results. Postprocedure 2D ECHO showed a good ejection fraction of 65%, ASD device in situ, no residual shunt across ASD, no mitral regurgitation, no tricuspid regurgitation, and no Pulmonary Arterial Hypertension (PAH) (Figure 7).
His post-ASD closure cardiac auscultation revealed a significant reduction in murmur intensity, however, features of hyperdynamic circulation were present. The post-procedure hospital stay was uneventful.
Discussion
Holt-Oram syndrome was first described in the 1960s by Mary Holt and Samuel Oram. They described a series of cases that presented with effort dyspnoea, ECG abnormalities, and deformity of the hands. A few of the cases described by them had survived until the 5th and 6th decade with no symptoms when they presented with complications suggestive of PAH. Cardiac catheterization was tried; however structural abnormalities of the heart prevented them from doing so. This is when they described this syndrome on the further investigation as having an ASD with an arrhythmia which may be accompanied by deformities in peripheral arteries and veins. Furthermore, the inheritance pattern was described as autosomal dominant [3].
In our case, the following findings fit into this syndrome, i.e., an upper limb deformity in the form of cavus deformity of the wrist with an absent thumb in the right hand. The forearm was short (indicating a lack of long bone). The patient also had a supernumerary digit in the left hand. There was the presence of ostium secumdum ASD confirmed with an ECHO [4]. There was no conduction block, however, the patient had significant tachycardia at rest and had multiple episodes of supraventricular tachycardia during the closure, which may indicate a conduction defect. This particular case could have a sporadic mutation instead of an autosomal dominant pattern as there was no positive family history and his ancestry also did not report any anomalies [5].
His normal stature, ophthalmological, skin, and dental examinations helped us to rule out Ellis-van Creveld syndrome. He did not have any thrombocytopenia which would have been fit for Thrombocytopenia-Absent Radius (TAR) syndrome. The patient after evaluation with radiographs did not have any axial skeleton or lower limb deformity. His IQ level was normal for his age [6]. The presence of features of an ostium secumdum type ASD, absent thumb and radius bone with normal development, and no other organ involvement are most suggestive of Holt-Oram syndrome.
Since the patient had a significant-sized ASD, we chose to close the defect. Since the patient was able to do his normal activities with his deformity, no intervention was planned to correct his upper limb deformity. Although routine abdominal sonography revealed right-sided renal agenesis, our patient did not have any clinical or biochemical evidence of renal failure. Considering Holt-Oram syndrome with unilateral renal agenesis, presentation is very rare. A similar case with unilateral renal agenesis and hypoplastic kidney has been reported in the literature [7,8].
The patient and his family were counseled about the nature of the disease, pattern of inheritance, and future familial involvement. However, children with severe limb shortening with limb shortening may benefit from prosthesis as well as physical and occupational therapy [9]. Procedures such as pollicization may also help these patients to bring functions of thumb. This article is to sensitize the medical fraternity regarding heart hand syndromes and to highlight interventions that could help rehabilitate the patient and as a measure to prevent future complications [10].
Conclusion
Holt-Oram syndrome-associated ASD can be closed with modern techniques of interventional cardiology with reduction of long-term complications and comfortable life. Correction surgery for deformities significantly improved the quality of life. Understanding such congenital syndromes and sensitizing the family to possible complications, the pattern of inheritance may also help in better familial planning.
Declarations
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Considerations
Written consent was obtained and signed by the legal guardians of the patient, for full disclosure while maintaining strict confidentiality in respect to the patient medical information and images under the approval of the Mahatma Gandhi Institute of Medical sciences (MGIMS), ethical committee (IRB-00003623).
References
- Al-Qattan, Mohammad M., and Hussam Abou Al-Shaar. "A novel missense mutation in the TBX5 gene in a Saudi infant with Holt-Oram syndrome." Saudi Medical Journal, Vol. 36, No. 8, 2015, pp. 980-82.
- Vanlerberghe, Clémence, et al. "Holt-Oram syndrome: clinical and molecular description of 78 patients with TBX5 variants." European Journal of Human Genetics, Vol. 27, No. 3, 2019, pp. 360-68.
- Holt, Mary, and Samuel Oram. "Familial heart disease with skeletal malformations." British Heart Journal, Vol. 22, No. 2, 1960, pp. 236-42.
- Bossert, T., et al. "Cardiac malformations associated with the Holt-Oram syndrome-report on a family and review of the literature." The Thoracic and Cardiovascular Surgeon, Vol. 50, No. 05, 2002, pp. 312-14.
- Cross, Stephen J., et al. "The mutation spectrum in Holt-Oram syndrome." Journal of Medical Genetics, Vol. 37, No. 10, 2000, pp. 785-87.
- Hoeffel, J. C., et al. "Malformations of the hand associated with congenital heart lesions." Australasian Radiology, Vol. 20, No. 1, 1976, pp. 72-82.
- EJ, Ferriols Gil, and Fayos Soler JL. "Holt-Oram syndrome. Presentation of two cases (author's transl)." Spanish Annals of Pediatrics, Vol. 15, No. 4, 1981, pp. 378-82.
Google Scholar Crossref
- Dasgupta, M. K., et al. "Unilateral hypoplastic kidney in a case of Holt-Oram Syndrome." Journal of Nepal Paediatric Society, Vol. 33, No. 1, 2013, pp. 77-79.
- Hafkemeyer, U., et al. "Holt-Oram syndrome. 3 case reports and their physical therapy, occupational therapy and technical orthopedic treatment." The Orthopaedist, Vol. 30, No. 4, 2001, pp. 226-30.
- Sletten, Lisa J., and Mary Ella M. Pierpont. "Variation in severity of cardiac disease in Holt‐Oram syndrome." American Journal of Medical Genetics, Vol. 65, No. 2, 1996, pp. 128-32.