Research - International Journal of Medical Research & Health Sciences ( 2022) Volume 11, Issue 12
Clinical profile of headache in ENT practice
Niveda Ramachandran*, Athithya S P and Anand K HNiveda Ramachandran, Department of Otorhinolaryngology, Saveetha Medical College and Hospital, Chennai, TamilNadu, India, Email: nivedhanive293@gmail.com
Received: 23-Oct-2022, Manuscript No. ijmrhs-22-78088; Editor assigned: 26-Oct-2022, Pre QC No. ijmrhs-22-78088 (PQ); Reviewed: 24-Nov-2022, QC No. ijmrhs-22-78088 (Q); Revised: 02-Dec-2022, Manuscript No. ijmrhs-22-78088 (R); Published: 20-Dec-2022
Abstract
Background: Headache is a common disorder or symptom experienced by every single person at least once in their lifetime. It is the main symptom in a wide variety of diseases, of which the ear, nose, and throat contribute only to a small number. The exact incidence of headache cases is not known, as all cases are not being reported. Though it may be mild pain in some patients, headache can also be a serious symptom of various life-threatening conditions. Method: This is a prospective study of 100 cases in the ENT department whose chief complaints were a headache. The patients within the age group of 12 years to 72 years were included in the study. Patients below and above this age group, patients with other comorbid, and patients with a history of recent head trauma were excluded from this study. A performed questionnaire was given to these patients and responses to the questionnaire were entered into an excel data sheet and the data was analyzed. Result: In this study, conducted in a tertiary care hospital, we found headaches to be common in the age group of 33 years to 42 years of age (30%), and affect females (59%) more than males (41%). The most common cause of headache diagnosed in patients coming to the ENT OPD was sinusitis (37%) diagnosed commonly by taking an x-ray of the paranasal sinuses. We found the most common triggering factor for the headache to be stress (25.6%). We also found the most common relieving factor for headaches to be medication (39.4%). And also some patients (38%) presenting to the ENT OPD with complaints of headaches had a previous history of sinusitis. 70% of people had disturbed sleep because of headache. Conclusion: Headache is a major complaint of patients coming to the ENT department. Headache can be treated by a general physician if it’s a primary type of headache. Some patients with associated ear, nose, and throat history are usually referred to ENT to look for any secondary etiology for the headache. The treatment of headache must usually be a multidisciplinary approach involving an ENT specialist, ophthalmologist, neurologist, psychiatrist, and general physician, which can be beneficial for the treatment and gives a better outcome for the patient.
References
Journals of Health Journals of Neurology Medication Articles Blog | Casino Sites in Netherlands Blog | Casino Sites in China Orthopedic Articles Urology Articles Real Estate in Arabic Country Blog | Casino Sites in Australia Blog | Best Betting Sites in Ukraine Real Estate in Australia Real Estate in Germany Blog | Car Insurance in USA Real Estate in Greece Blog | Casino Sites in Indonesia Real Estate in Indonesia Blog - Find Lawyer in Virginia Real Estate in India Blog | Casino Sites in India Real Estate in MalaysiaKeywords
Headache, Primary headache, Secondary headache, Sinus headache
Introduction
Headache is defined as a painful sensation or any unpleasant feeling in the region of the head above the supraorbital line that can range from sharp to dull and may be accompanied by other symptoms [1,2]. Only a small percentage of the vast number of people affected are properly diagnosed by medical personnel [3]. It is one of the most under-recognized, underestimated, and under-treated conditions. Headache is a symptom produced by the nervous system when it perceives a threat and as such is sometimes considered to be a protective physiology of the nervous system according to Moskowitz.
Classifying headaches is not easy because there are a lot of types and several causative factors or triggers for each type. The classification by the IHS (International Headache Society) is called the ICHD- International classification of headache disorders (3 rd edition) [4]. The International Classification of Headache Disorders (ICHD) classification now accepted by the WHO classifies headaches mainly as primary headaches and secondary or symptomatic headaches. Primary headaches occur without the involvement of any other cause, and no actual pathologic condition can be identified [5]. Secondary headaches are caused by some other factor at play; that is, when the cause of the headache is a definable pathologic process, the headache is diagnosed as a secondary headache
Primary headache types include major categories which are migraine tension-type headache, Trigeminal autonomic Cephalgias, and the last being other primary headache disorders [6-8]. Secondary headaches include trauma or injury to the head or neck, cranial or cervical vascular disorders, non-vascular intracranial disorders, substance withdrawal, infection, a disorder of homeostasis, cranial neuropathies, and other facial pain, with the last being headache attributed to psychiatric disorders.
Fortunately, the majority of patients who visit their primary physician for an evaluation have a primary headache disorder. The diagnosis of some life-threatening conditions that present with headaches, such as meningitis, brain hemorrhage, glaucoma-caused headache, and acute purulent sinusitis, is usually straightforward by the respective specialists [9-11]. When a headache is chronic, recurrent, and unaccompanied by other vital signs of the underlying condition, it is considered the most difficult medical problem, and the treating physician should perform a complete physical and neurological examination.
Method
Aim:
To evaluate the most common presenting cause of headache in patients presenting to the ENT OPD.
Objective
To clinically assess the patients with complaints of headache and assess the risk factors, relieving factors and categorize the patients and quick treatment.
A total of 100 patients were selected who presented in the ENT OPD in save the medical college for 6 months with the primary complaint as headache
Sample size calculated using the formula
Sampling technique: Nonprobability convenience method Source of data.
Patients for the study were collected from ENT OPD Saveetha medical college and hospital, Thandalam.
Inclusion Criteria
• Age groups from 12 years to 72 years were included in the study.
• Any patient coming to the ENT OPD for evaluation of headache.
Exclusion Criteria
Age groups children less than 12 years as the history of the child cannot be reliable and can lead to false positive results.
Patients with Co-Morbidities
Patients with a history of recent head trauma as the headache could more likely be due to impact injury not related to primary headache. A questionnaire was given to every patient who fit the criteria. The questionnaire contains questions to determine the factors responsible for headaches and their prevalence based on gender, age, intensity, duration, frequency, site of headache, and sleep habits of the patient. Factors that aggravate and relieve headaches according to every individual patient were also collected. Any past or present medical disorder, history of head trauma, use of self-medication, and the number of visits made to a specialist were also documented. The clinical profiling was based on the main risk factor for the cause of the headache, the number of times the patient visited the doctor for the same complaints to various specialties.
Every patient who came in with a headache had a complete ENT and neurological examination done. All the data collected was entered into a spreadsheet, and the data were analyzed according to age distribution, gender distribution, and the common diagnosis for the secondary etiology of the headache. Headache disrupts a patient's lifestyle, such as sleep disruptions and missed work. The most common headache aggravating and relieving factors
Result
The study comprises patients coming to the ENT OPD for the evaluation of headaches, 100 patients from the age group of 12 to 72 were included in the study (Figure 1-6)(Table 1-4)
| Headache effect on work | Percentage of people |
|---|---|
| Yes | 64% |
| No | 36% |
| Headache effect on sleep | Percentage of people |
|---|---|
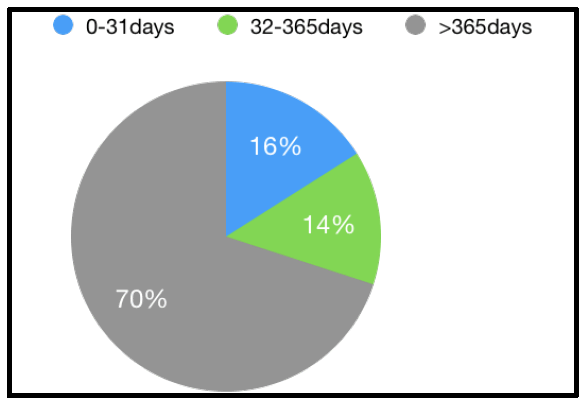
| Yes | 70% |
| No | 30% |
| Sinusitis history | Percentage of people |
|---|---|
| Yes | 38% |
| No | 62% |
| Location of the headache | Percentage of people |
|---|---|
| Forehead | 30% |
| Temporal | 20% |
| Retro-orbital | 12% |
| Occipital | 8% |
| Entire head | 14% |
| Neck | 6% |
| Sides | 10% |
Discussion
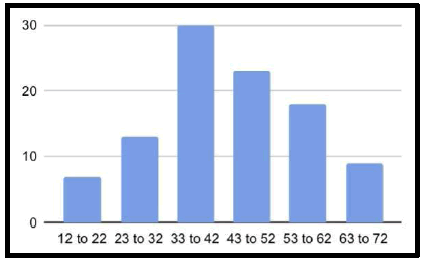
The study was conducted in a tertiary care hospital in Thandalam, and the objective of the study was to know the incidence of patients coming to the ENT specialist with complaints of headache. The age group included in the study was from 12 years to 72 years and was divided into 6 categories: 12 years to 22 years (7%), 23 years to 32 years (13%), 33 years to 42 years (30%), 43 years to 52 years (23%), 53 years to 62 years (18%), and 63 years to 72 years (9%), with a maximum of 30% found in the category of 33 years to 42 years of age. Many studies have found that the incidence of headaches decreases after the age of 40.
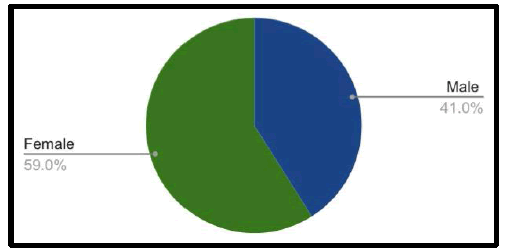
According to the study, females suffer from headaches more commonly than males, with the incidence being 54% in females and 46% in males in this study. Many epidemiological studies have also found that women have a higher prevalence of headaches [12-14].
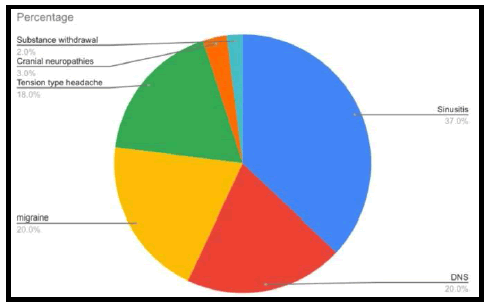
Sinusitis was found to be the most common diagnosis in patients presenting with headache complaints or referred from other departments to rule out secondary etiology at a tertiary care center's ENT department (37%). Sinusitis can be diagnosed by taking and examining the paranasal sinuses [15,16]. DNS (20%), migraine (20%), tension-type headache (18%), cranial neuropathies (3%), and substance withdrawal (2%) were the other causes of headache encountered.
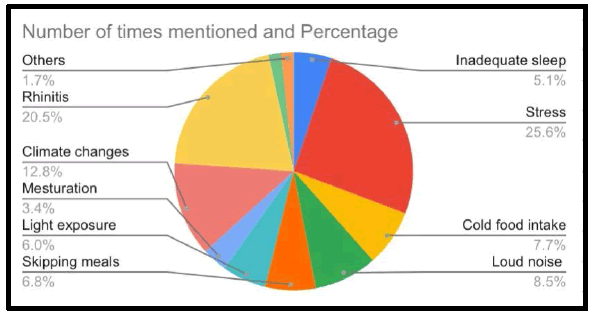
Among the vast list of triggering factors for the headache, the most common was found to be stress (25.6%). Stress is the most common trigger for headaches in various studies as well [12,13]. Rhinitis (20.5%) was found to be the second most common triggering factor. Other triggering factors include climate changes (12.8%), loud noises (8.5%), cold food intake (7.7%), skipping meals (6.8%), light exposure (6%), inadequate sleep (5.1%), menstruation in female patients (3.4%), and others (1.7%).
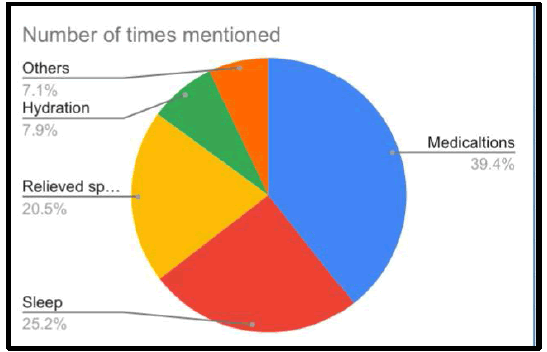
The relieving factor was most commonly found to be medications (39.5%). 13.25% of people were relieved of headaches with good sleep. Some people had spontaneous relief from the headache (20.5%) or mostly didn't know the actual cause of relief for the headache. Proper hydration was also a specific relieving factor for a few patients (7.9%).
A few of the patients were also referred to other specialists in the hospital, like ophthalmology, neurology, psychiatry, and general medicine, for future management of the headache, and patients were referred from these specialty departments to ENT for the evaluation of headaches of secondary Etiology.
Conclusion
Headache is one of the most common complaints among people of all ages. According to many studies, most headaches have a trigger factor and a definitive relieving factor, which are stress and medications, respectively. It is more common in the female gender than in the male gender. Most of the patients presenting to a physician suffer from a muscular type of headache or a vascular type of headache, unlike other people diagnosed with sinusitis either by the treating physician or by self-diagnosis. Hence, most of the patients who come with the complaint of a headache can be treated by a general physician. At the same time, a secondary etiology for the cause of the headache must also be ruled out.
The treatment of headache must usually be a multidisciplinary approach involving an ENT specialist, Ophthalmology, Neurology, Psychiatry, and a general physician, which can be beneficial for the treatment of the patient.
Declarations
Conflict of Interest
The authors’ declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article
References
- Ahmed, Fayyaz. "Headache disorders: differentiating and managing the common subtypes." British journal of pain, Vol. 6, No. 3, 2012, pp. 124-32.
Google Scholar Crossref - Aromaa, Minna, Matti Sillanpää, and Hillevi Aro. "A population-based follow-up study of headache from age 7 to 22 years." The Journal of Headache and Pain, Vol. 1, No. 1, 2000, pp. 11-15.
Google Scholar - Stovner, L. J., et al. "The global burden of headache: a documentation of headache prevalence and disability worldwide." Cephalalgia, Vol. 27, No. 3, 2007, pp. 193-10.
Google Scholar Crossref - Arnold, Marcel. "Headache classification committee of the international headache society (IHS) the international classification of headache disorders." Cephalalgia, Vol. 38, No. 1, 2018, pp.1-211.
Google Scholar Crossref - Jensen, R., et al. "European principles of management of common headache disorders in primary care." Journal of Headache and Pain, Vol. 8, 2007, p. 3.
Google Scholar Crossref - Ahmed, Fayyaz. "Headache disorders: differentiating and managing the common subtypes." British journal of pain, Vol. 6, No. 3, 2012, pp. 124-32.
Google Scholar Crossref - Hildreth, Carolyn J., Cassio Lynm, and Richard M. Glass. "Migraine headache." Jama, Vol. 301, No. 24, 2009, pp. 2608-08.
Google Scholar - Goadsby, P. J., et al. "The changing face of chronic migraine: who to treat? How to treat." BMJ Neurol, 2010, pp. 1-4.
Google Scholar - Cady, Roger K., and Curtis P. Schreiber. "Sinus headache: a clinical conundrum." Otolaryngologic Clinics of North America, Vol. 37, No. 2, 2004, pp. 267-88.
Google Scholar Crossref - Schreiber, Curtis P., et al. "Prevalence of migraine in patients with a history of self-reported or physician-diagnosed sinus headache." Archives of internal medicine, Vol. 164, No. 16, 2004, pp. 1769-72.
Google Scholar Crossref - Cady, Roger K., and Curtis P. Schreiber. "Sinus headache: a clinical conundrum." Otolaryngologic Clinics of North America, Vol. 37, No. 2, 2004, pp. 267-88.
Google Scholar Crossref - Bahra, Anish, Arne May, and Peter J. Goadsby. "Diagnostic patterns in cluster headache." Frontiers In Headache Research, Vol. 9, 1999, pp. 61-65.
Google Scholar - Sarlani, Eleni, et al. "Chronic paroxysmal hemicrania: a case report and review of the literature." Journal of orofacial pain, Vol. 17, No. 1, 2003, pp. 74-78.
Google Scholar - Bahra, Anish, Arne May, and Peter J. Goadsby. "Cluster headache: a prospective clinical study with diagnostic implications." Neurology, Vol. 58, No. 3, 2002, pp. 354-61.
Google Scholar Crossref - Osguthorpe, J. David. "Adult rhinosinusitis: diagnosis and management." American family physician, Vol. 63, No. 1, 2001, p. 69.
Google Scholar - Cady, Roger K., et al. "Sinus headache: a neurology, otolaryngology, allergy, and primary care consensus on diagnosis and treatment." Mayo Clinic Proceedings, Vol. 80. No. 7, 2005, pp. 908-16.
Google Scholar Crossref