Research - International Journal of Medical Research & Health Sciences ( 2021) Volume 10, Issue 2
Cystadenofibroma of the Ovary: An Uncommon Ovarian Neoplasm
Lalit Banswal1, Aditya Manke1, Vijaylaxmi Ganorkar1, Yogesh Kumar2, Rahul Patil3, Samadhan Pawar4, Yasam Venkata Ramesh5 and Raj Nagarkar1*2Department of Obstetrics and Gynecology, Ganorkar Hospital, Nashik, Maharashtra, India
3Department of Pathology, HCG Manavata Cancer Centre, Nashik, Maharashtra, India
4Department of Radiology, HCG Manavata Cancer Centre, Nashik, Maharashtra, India
5Department of Academics, HCG Manavata Cancer Centre, Nashik, Maharashtra, India
Raj Nagarkar, Department of Surgical Oncology, HCG Manavata Cancer Centre, Nashik, Maharashtra, India, Tel: 9823061929, Email: academics@manavatacancercentre.com
Received: 30-Dec-2020 Accepted Date: Feb 11, 2021 ; Published: 18-Feb-2021
Abstract
Among the wide variety of ovarian neoplasms, ovarian cystadenofibroma is a rare benign neoplasm. In the present study, we report two such rare cases, where initial pre-operative imaging studies and frozen section specimen were in favor of malignancy. However, biopsy studies of the same revealed it to be benign cystadenofibroma. Both the patients successfully underwent hysterectomy with bilateral salphingo-oophorectomy.
Keywords
Cyst, Adenofibroma, Ovary, MRI, Histopathology
Introduction
Ovarian Cystadenofibromas (OCAF) are very rare, often asymptomatic, benign epithelial ovarian lesions, accounting 1.7% of all benign ovarian neoplasms [1]. It can occur at any age, but is most commonly observed in women aged between 40 to 60 years old. Its diverse structures are composed of cysts or glands or solid fibrotic tissues. These neoplasms are classified into several histological subtypes, according to epithelial types as clear cell, mucinous, endometrioid, serous, and mixed [2]. Further, they were classified as benign (epithelial, stromal, and germ cell), borderline, and malignant neoplasms depending upon the degree of epithelial proliferation and fibroblastic stromal component [3]. The main concern in these neoplasms is their similarity with other malignant lesions of the uterus. So, preoperative differential diagnosis plays a crucial role in distinguishing benign OCAF from malignant neoplasms. Here we report, two uncommon cases of benign cystadenofibroma involving bilateral ovaries, treated with hysterectomy with bilateral salphingo-oophorectomy.
Case Report
We have retrospectively collected and analyzed the data from our electronic medical records of the patients diagnosed with cystadenofibroma, who received treatment in our center from 1st January 2018 to 31st January 2020. We found only 2 such cases, confirming the rarity of these types of ovarian neoplasms.
Case 1
A 35-year old female presented complaining about abdominal pain and discomfort for 3 months. No history of malignancy in the family. Hormonal status was normal. Pelvic examination was positive for abdominal mobile mass. CT-Scan revealed bilateral large ovarian masses with solid components. Diagnostic laparoscopy and frozen biopsy have confirmed the diagnosis as benign cystadenofibroma.
Case 2
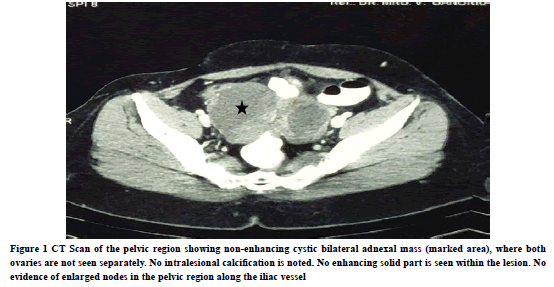
A 49-year old female was presented at our hospital, with a history of lower abdominal pain. CT scan has shown anterior-posterior 8.5 × 8.2 × 5.7 cm irregular mixed large cystic and solid component, with mild enhancement and calcification (Figure 1).
Figure 1. CT Scan of the pelvic region showing non-enhancing cystic bilateral adnexal mass (marked area), where both ovaries are not seen separately. No intralesional calcification is noted. No enhancing solid part is seen within the lesion. No evidence of enlarged nodes in the pelvic region along the iliac vessel
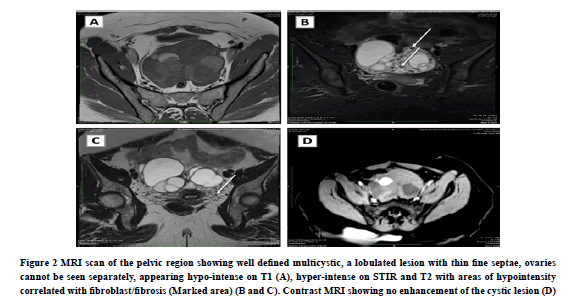
MRI scan (Figure 2) has shown a well-defined multilobulated, multicystic, altered signal intensity in the bilateral adnexal region, where both the ovaries were not seen separately. The right adnexal lesion measures 7.1 cm × 6.9 cm in size and the left adnexal lesion measures 6.1 cm × 4.3 cm in size which was appearing hypo-intense on T1WI, and hyper-intense on T2WI. Internal thin septations were noted within the lesion, measuring 1 mm-2 mm in size. The inferior aspect of the lesion was showing a solid curvilinear component without any demonstrable enhancement after the post-contrast scan. We have also observed few hypo-intense signal intensity foci (T2WI) in the inferior aspect of the lesion, appearing as a black sponge image. On a dedicated CT cut, no calcifications were noted. So above foci may be representing the possibility of fibrosis part. Rest uterus was showing intramural and sub-mucosal fibroids in the body.
Figure 2. MRI scan of the pelvic region showing well defined multicystic, a lobulated lesion with thin fine septae, ovaries cannot be seen separately, appearing hypo-intense on T1 (A), hyper-intense on STIR and T2 with areas of hypointensity correlated with fibroblast/fibrosis (Marked area) (B and C). Contrast MRI showing no enhancement of the cystic lesion (D).
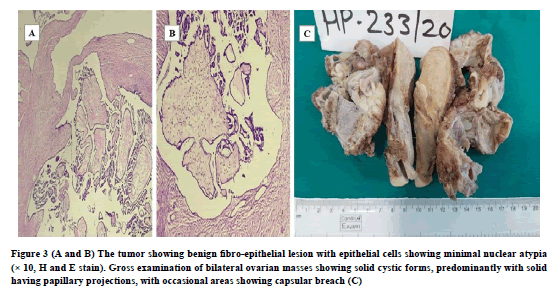
On diagnostic laparoscopy, uterus enlargement with heterogeneous attenuation with a 3.6 × 3.0 × 2.8 cm size nodular lesion was observed in the left side postero-lateral wall. Operational findings observed bilateral ovarian masses with pelvic peritoneal and sub-diaphragmatic peritoneal deposits. The frozen section specimen was suspicious of malignancy. However, biopsy studies of the same revealed it to be benign cystadenofibroma (Figure 3).
Figure 3. (A and B) The tumor showing benign fibro-epithelial lesion with epithelial cells showing minimal nuclear atypia (× 10, H and E stain). Gross examination of bilateral ovarian masses showing solid cystic forms, predominantly with solid having papillary projections, with occasional areas showing capsular breach (C).
On gross examination, bilateral ovarian masses were externally showing shiny capsules with lobulations, with occasional areas showing capsular breach. On sectioning, the ovarian mass was found to be an admixture of solid and cystic parts, but a predominantly solid part. Cysts were filled with hemorrhagic fluid. Overall, areas of necrosis were not seen.
On microscopy, the tumor has shown a fibroepithelial lesion with a large stromal component. Small cysts were also noted with thin papillary fibrous septae lined by epithelial cells. Cytological atypia was minimal. Mitosis was 0-1/50 HPF. Depending upon the histological features, a diagnosis of cystadenofibroma was made. The patient underwent a hysterectomy with bilateral salphingo-oophorectomy.
Discussion
Cystadenofibroma of the ovary is a very rare benign neoplasm variant with the least possibility of malignant potential. However, surgical intervention is highly recommended. They generally form from the ovarian epithelial surface and this epithelial component secretory activity will determine the nature of the neoplasm (liquid or semisolid or solidstate) [4]. Depending on the fibrous stroma, they are further classified into various subtypes (i.e., cystic or fibrous).
The usual complaints of the patients on presentation are abdominal pain and discomfort in the pelvic or lower abdominal region with a palpable mass. In advanced stages, patients will experience dysmenorrhea, dysuria, postmenopausal bleeding, pelvic pressure symptoms, increased abdominal girth, rectal urgency, and vaginal bleeding [3,5-7].
In both cases presented, the patients presented with multiple benign fibroepithelial ovarian lesions, showing capsular breach. The initial diagnosis was strongly suspecting the ovarian malignancy because of the multiple cystic masses. CT and MR imaging have strongly confirmed the cystic mass lesions arising from bilateral adnexal regions, separated by thick septa. They are typically large multicystic, multilobulated, with altered signal intensity displaying the characteristic hypo-intense on T1 and hyper-intense on T2 weighted sequences and a black sponge aspect. These complex cystic, as well as differentiated septal areas, made the case as suspected to be malignant with differential diagnosis in favor of cystic neoplasms and granulosa cell neoplasms.Many investigations have reported that this type of neoplasms could be misinterpreted and wrongly diagnosed as a malignancy in the pre-operative imaging studies [3,8].
The first case of such clinical misinterpretation was reported by Hughesdon in 1949, as published in proceedings of the royal society of the medicine, where a patient with bilateral ovarian neoplasm was misinterpreted as endometriosis [9]. In another study reported by Song, et al., among 29 cases, 14 cases (48.3%) were incorrectly characterized as malignant neoplasms on imaging [8]. Wasnik and Elsayes also reported the misinterpretation and appearance of complex, cystic-solid appearing masses of OCAF resembling malignant neoplasm, on imaging [1]. In another report by Samarth, et al. the clinical and radiological findings of bilateral ovarian mass with ascites were in the favor of malignancy or infective process [3].
In all the above cases, imaging data was misguided and misinterpreted, giving a false-positive impression of benign neoplasm as malignant neoplasm which was proven to be wrong by further histopathological examination of specimens [4-7]. To the surprise, in many cases, even during the surgery, the gross appearance of the neoplasm appears to be as malignant neoplasm.
On the contrary, some case reports are in favor of MRI as an essential modality for pre-operative diagnosis in determining such rare neoplasms based on the signal intensity of T2-weighted images [2].
Overall, to avoid any such diagnostic errors and to save the patient from unnecessary extensive surgery/surgical procedures, always intraoperative frozen section diagnosis and histopathological examination is preferred. Whereas knowing this rare OCAF neoplasm is very helpful and important to all the clinicians and pathologists from the clinical point of view and to save the patient from unnecessary extensive surgical related trauma.
Conclusion
Since cystadenofibroma of the ovary is a benign tumor with a rare potential for malignant transformation. We believe that when treating young patients, the conservative surgical approach is essential. The intraoperative frozen section may be very helpful in many of these cases. Because this tumor has malignant radiological features and since it may appear as malignant intra-operatively (due to its numerous papillary protrusions with capsular breach), it is well advised to be aware of the possibility of a benign tumor before an aggressive surgical approach is selected.
Declarations
Conflicts of Interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Financial Disclosure
None.
Ethical Approval
No ethical approval was necessary for a case report.
Informed Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
References
- Wasnik, Ashish, and Khaled Elsayes. "Ovarian cystadenofibroma: A masquerader of malignancy."The Indian Journal of Radiology and Imaging,Vol. 20, No. 4, 2010, pp. 297-99.
- Lee, Dae Hyung. "A case of mucinous cystadenofibroma of the ovary."Case Reports in Obstetrics and Gynecology,Vol. 2014, 2014.
- Shukla, Samarth, et al. "Serous adenofibroma of ovary: An eccentric presentation."Journal of Cancer Research and Therapeutics,Vol. 11, No. 4, 2015, p. 1030.
- Montoriol, P-F., et al. "Fibrous tumours of the ovary: Aetiologies and MRI features."Clinical Radiology,Vol. 68, No. 12, 2013, pp. 1276-83.
- Dillon, Katrina, et al. "Ovarian serous cystadenofibroma with stromal sex cord elements: Report of a unique case."International Journal of Gynecological Pathology,Vol. 25, No. 4, 2006, pp. 336-39.
- Maciel, R., et al. "Adenofibroma in a young patient: A rare entity in an uncommon age."Case Reports in Obstetrics and Gynecology,Vol. 2013, 2013.
- Paşaoğlu, Ö., et al. "Benign clear cell adenofibroma of the ovary."Gynecologic and Obstetric Investigation,Vol. 64, No. 1, 2007, pp. 36-39.
- Cho, Song-Mee, et al. "CT and MRI findings of cystadenofibromas of the ovary."European Radiology,Vol. 14, No. 5, 2004, pp. 798-804.
- Sharman, Albert, and A. M. Sutherland. "A case of serous adenofibroma of the ovary."BJOG: An International Journal of Obstetrics and Gynaecology,Vol. 54, No. 3, 1947, pp. 382-83.