Research - International Journal of Medical Research & Health Sciences ( 2021) Volume 10, Issue 5
Emerging Role of Vitamin D in Women’s Health
Shipra Jha* and Nahid SiddiquiShipra Jha, Amity Institute of Biotechnology, Amity University, Noida, Ghaziabad, India, Tel: 8860006941, Email: sjanvi79@gmail.com
Received: 21-Apr-2021 Accepted Date: May 18, 2021 ; Published: 25-May-2021
Abstract
Vitamin D being a key nutrient also considered as a steroid prohormone, can be acquired by sun exposure and food sources with enhanced Vitamin D. Earlier, the function of Vitamin D was being restricted to maintenance of calcium and phosphorus levels and bone health. In this review, the focus is reflected on the Hypovitaminosis D and harmful consequences in the health of females and the disorders which are associated with Hypovitaminosis D among women aged 15 years and above. The advantage of Vitamin D to pregnant women is of major significance to fetal programming as well as to the mother’s health. Hypovitaminosis D, a great pandemic issue, is of great interest and concern among researchers, clinicians, and nutritionists as it is prevalent in almost all age groups- infants, girls, pregnant and lactating women, adult women, and elderly women. The effective and inexpensive approach of Vitamin D utilization being a therapeutic agent is of great importance in treating Vitamin D deficiency-associated disorders and increasing the Vitamin D statuse.
Keywords
Vitamin D, Hypovitaminosis D, Pregnancy, Obesity, Cancer, Vitamin D supplementation
Introduction
Vitamin D, known as a ‘sunshine vitamin’ as it is obtained from sunlight exposure and foods and supplements fortified with Vitamin D. It performs remarkable and important functions in women’s health. Various newer therapies are emerging with new concepts as a topic of great interest [1-3].
Vitamin D is considered a steroid prohormone as well as an indisputable nutrient. It can be synthesized by the skin. Poor dietary intake or absorption and poor sunlight exposure can lead to inadequate serum 25-OHD levels. Vitamin D was discovered as an important nutrient as a remedy for rickets-a disorder that weakens the bones, highly prevalent in the United Kingdom. It was noted that rickets can be treated/prevented when cod liver oil and sunlight exposure is provided [4,5]. For a prolonged period, Vitamin D’s purpose is thought to be restricted only in maintaining bone health metabolism and Calcium and phosphorus levels. As the Vitamin D Receptors (VDRs) are present on various body organs such as the brain, skin, pancreas, breast, colon, and prostate cancer cells and immune cells; so it acts as a hormone and the new functions of Vitamin D, associated with these organs, are emerging which are beyond bone health [6].
About 1 billion people are suffering from Hypovitaminosis D, have serum Vitamin D concentrations low in the blood. Beyond 40% of the reproductive age women found to have inadequate levels of Vitamin D. Hypovitaminosis D occur due to fat malabsorption syndromes, use of anticonvulsants and glucocorticoids, chronic kidney disease, obesity, elder women having a medical record of falls or fractures, musculoskeletal disease, hepatic failure and cancer [7]. Hypovitaminosis D is an important pandemic matter of problem and can be defined as when serum 25-(OH) D levels are found below 20 ng/m1 in the blood. It is highly observed in almost all age groups-infants, girl children, pregnant and lactating women, adult women, and elderly women [8].
Literature Review
Classification of Vitamin D Deficiency
It is categorized into three groups: Vitamin D deficiency, Vitamin D insufficiency, and Vitamin D sufficiency. Vitamin D insufficient is when serum Vitamin D levels are found to be in between (20-30) ng/ml (Table 1). Vitamin D sufficiency group found to have serum Vitamin D levels above 30 ng/ml in blood [9].
Table 1: Vitamin D deficiency categorization depending upon 25-hydroxyvitamin D concentration
| 25-(OH)D concentration (ng/m1) | Vitamin D status |
| Lower than 20 | Deficiency |
| Between 20-30 | Insufficiency |
| Above 30 | Sufficiency |
| Above 150 | Risk of toxicity |
Incidence
About 80% of the healthy population is turned as Vitamin D deficient i.e. below 20 ng/m1 serum 25-(OH) D is found whereas approx. 40% are severely deficient i.e. less than 9 ng/ml serum 25-(OH) D is found. Hypovitaminosis D can be found in almost one out of three infants of age 1-6 months due to the lower levels of 25-hydroxyVitamin D in mothers [10].
Causes of Hypovitaminosis D
Deficiency can be highly observed in people with dark pigmentation, women who use sunscreen lotions as they are getting more aware of skin cancer, people suffering from milk allergies or are lactose intolerant, and restricted to a vegan diet. Preference for cold drinks and juices over milk makes children Vitamin D deficient. People living in urban areas spend more time working and are involved in less physical activity get inadequate sun exposure and become obese or overweight and in turn, become Vitamin D deficient [11]. Dark-skinned individuals are usually more Vitamin D deficient than light-skinned people due to the presence of more melanin in dark-skinned people, which acts as a natural sun protector and leads to less generation of Vitamin D by the skin. Hypovitaminosis D is also affected via. seasonal changes as during winter Vitamin D levels are observed to be low in individuals as compared to summers. Poverty and illiteracy are also some of the reasons as people are not much aware of Vitamin D sources and the importance of a balanced diet. Social and religious customs also play a role as women and their infants usually stay indoors, so they are less exposed to the sun and susceptible to be Vitamin D deficiency. Individuals who wear more clothing such as burqas are also susceptible to Vitamin D deficiency as they receive less sunlight exposure [12].
Vitamin D has two major forms-Vitamin D2 i.e. (ergocalciferol), which is acquired by intake of food of plant origin, and Vitamin D3 i.e. (cholecalciferol) which is acquired by intake of food of animal origin. We can get Vitamin D by intake of food sources such as fish oil, some fish includes salmon, tuna, sardines, cod liver oil, fortified food with Vitamin D supplemented milk, yogurt, biscuits, egg, soy products, orange juice, cereals, and infant formula [13].
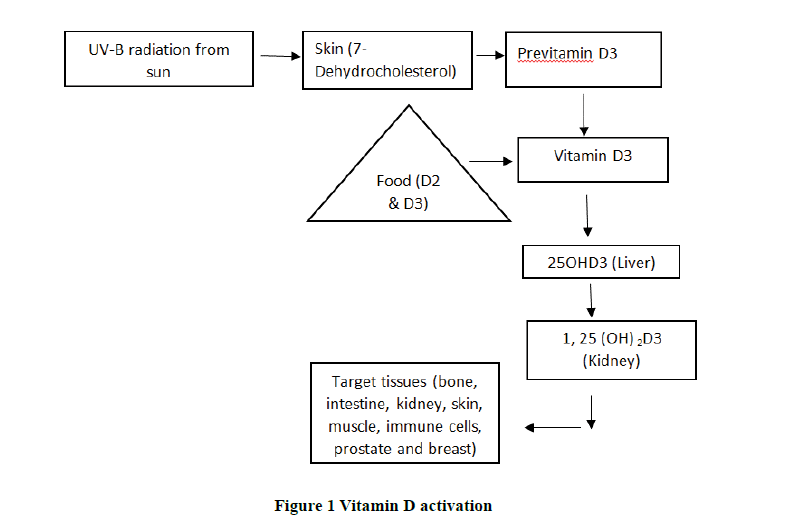
Activation of Vitamin D
Vitamin D3 is formed in the body by absorbing UV-B rays from sunlight exposure. Vitamin D3 formation occurs between 10 AM to 3 PM. Vitamin D3 which is obtained from sunlight exposure is not biologically active. It gets activated due to the presence of 7-Dehydrocholesterol (7-DHC) in human skin which converts it into pre-Vitamin D3. It is transported to the liver and undergoes a hydroxylation reaction, where it gets converted to 25-hydroxy Vitamin D [25-(OH) D]. Further, it is carried to kidneys and undergoes another hydroxylation reaction, gets converted to 1, 25-dihydroxyvitamin D [1,25-(OH)2 D3), biologically active form, gets transported to different target tissues upon binding with its VDRs (Figure 1).
Vitamin D testing can be done by measuring the serum 25-hydroxyVitamin D [25-(OH) D] concentration in the blood, which is the best indication of Vitamin D levels.
Vitamin D Requirement
According to the Institute of Medicine (IOM), Recommended Dietary Allowances (RDA) specified for different age groups is varied. For infants: 400 IU (10 μg), for children and adults (up to 70 years): 600 IU (15 μg) and for elders (over 70 years): 800 IU (20 μg) is recommended [14-16]. According to Endocrine Society, RDA for children is 600- 1000 IU (15 μg-25 μg) and for adults: 1500-2000 IU (37.5 μg-50 μg) is recommended (Table 2).
Table 2: Vitamin D intake requirements (by Institute of Medicine and Endocrine Society)
| Age | Institute of Medicine (IOM) Recommendations | Endocrine society Recommendations | ||
| RDA (IU/day) | Upper limit (IU/day) | Daily recommendations (IU/day) | Upper limit (IU/day) | |
| Infants (0-12 months) | 400 IU (10 µg) | 1000-1500 | 400-1000 | 2000 |
| Children and adults (up to 70 years) | 600 IU (15 µg) | 2500-4000 | 600-1000 | 4000 |
| Pregnant and lactating women | 600 IU (15 µg) | 4000 | 1500-2000 | 4000 |
| Elders (>70 years) | 800 IU (20 µg) | 4000 | 1500-2000 | 4000 |
Vitamin D Toxicity/Hypervitaminosis D
It can occur if the use of Vitamin D supplements is in excess i.e. above 4000 IU. According to the Institute of Medicine (IOM) the Upper Level (UL) intake for infants is 1000 IU/day-1500 IU/day, for children, adults, pregnant women, and elders: 2500 IU/day-4000 IU/day [17-19]. If serum Vitamin D level is above 150 ng/m1, it can lead to further problems in the body such as-Hypercalcemia (increased concentration of calcium in the blood) and can cause Hypercalciuria and Hyperphosphatemia (increased level of phosphorus in blood). In the long term, it can lead to the hardening of vessels and tissues and harm to the heart, blood vessels, and kidneys. In WHI, postmenopausal women who consumed Ca (1000 mg/day) and Vitamin D supplements (400 IU) consumed for seven years, were found to be a 17% greater possibility of renal stones [20-24].
Vitamin D controls the Ca levels in the body. But the new functions are coming forward with the knowledge of various functions performed by Vitamin D on different body organs [25-27]. Its inadequate level might lead to problems such as osteoporosis, Rheumatoid arthritis, Multiple sclerosis, Hypertension, Cardiovascular Diseases, obesity, psoriasis, psychiatric disorders, and problems in pregnancy-which is related to Hypovitaminosis D [28-32].
Classical Roles
Vitamin D regulates growth and development in the body. From the beginning of pregnancy till late pregnancy, absorption of intestinal calcium doubles but a very low amount gets transferred to the fetus. For fetus development, calcium requirement is met by biological changes in the mother’s body with an increased level of calcium. It increases calcium absorption to accelerate the blood calcium levels during the growth and pregnancy period by acting on the intestine. It works with parathyroid hormone to boost calcium reabsorption in the kidney and to release calcium from bones if this elevated intestinal absorption is inadequate in restoring the normal calcium levels. Vitamin D is involved in the skeletal system as it acts on the intestine, kidney, and skeleton to maintain calcium homeostasis. In extra-skeletal effects, its roles are emerging as it acts on skin, pancreas, placenta, prostate, breast, and colon cancer cells, heart, gonads, and the cells involved in maintaining the immune system [33].
Non-Classical Roles in other Disorders
Problems in pregnancy: Vitamin D levels are elevated during pregnancy and it is one of the vital nutrients in the development of the child. Hypovitaminosis D is highly prevalent in pregnant and lactating women [34-36]. In the United States, around 33% of the pregnant ladies are found to have reduced levels of Vitamin D. During pregnancy, calcium level gets reduced and hormones such as parathyroid hormone and lactogenic hormone get increased, as calcium is required by offspring and Ca is also get eliminated in the urine, which leads to deficiency both in mother and baby [37]. Parathyroid hormone acts as a calciotropic hormone that helps to regulate calcium levels during pregnancy. Vitamin D aids in the growth and maturation of the placenta, baby’s implantation, and prenatal programming. Infants are susceptible to the threat of rickets and other birth abnormalities in the baby. It helps in restoring the skeletal functions of the mother and in the production of skeletal functions in newborns. Deficiency can abruptly damage these functions. Deficient mothers are prone to pain in muscles and bones [38].
In a preterm birth, a baby is born earlier without the completion of the gestation period (before 37 weeks). Every year around fifteen million infants have preterm birth and responsible for the death of the baby and also suffer from other medical problems. Vitamin D supplementation to adequate levels can decrease the chances of preterm birth by 40%. In a study, there were five hundred women about twelve weeks pregnant were enrolled. They were given Vitamin D-400 IU/day, 2000 IU/day, or 4000 IU/day. And it is found that women who got 4000 IU/day are at reduced risk of preterm labor, delivering babies who are premature, and getting infections. Hypervitaminosis D/Vitamin D toxicity is mostly unusual however, can be treated easily. A pregnant woman deficient in Vitamin D has to suffer from hypertension in which the blood pressure is found to be elevated and can lead to preeclampsia and gestational diabetes (increased blood sugar levels in the blood) and they are more susceptible to deliver a baby via cesarean section. Preeclampsia affects around 3%-6% of pregnancies [39].
It can occur due to impairment in the maintenance of calcium levels and the oxidative stress generated in the placenta. Vitamin D serves a significant function in controlling the inflammation of the placenta. In a study, the association of lower levels of Vitamin D and bacterial vaginosis is shown to be interrelated. Higher levels of Vit. D can be effective in preventing bacterial vaginosis and thereby preterm labor pain by influencing the antimicrobial response [40].
A fetus gets Vitamin D via the passage of the placenta, so it is completely relying on the mother for the requirements of Vitamin D. If a mother has inadequate levels of Vitamin D, the child will be ultimately Vitamin D deficient. A baby delivered by Vitamin D deficient mother can also suffer from various problems as they receive poor Vitamin D levels which can lead to a reduction in bone mineralization and birth weight. Vitamin D deficient child might have to suffer from several other diseases such as Type I Diabetes, Asthma, stuffiness in the nose i.e. Rhinitis. If a woman has inadequate levels of Vitamin D, it can lead to a reduction in the period of pregnancy, which ultimately affects the growth and development of bones of the child [41].
In a case-controlled study, women having lower levels of Vitamin D i.e. <15 ng/ml were found at a greater risk of delivering a baby via. C-section then the women had higher Vitamin D levels-above 15 ng/ml [42]. In a meta-analysis study of approx. 463 women, women who consumed low Vitamin D intake were found to deliver a child having less than 2500 g weight. A study stated that the Vitamin D supplementation of 2400 IU/day to pregnant ladies was found to be effective in maintaining blood glucose and insulin levels.
Obesity: Obesity is the increase of fat mass in the body and is one of the major global issues. It is one of the main causes responsible for an individual to be Vitamin D deficient. More weight results in more Vitamin D requirement of the body [24,43]. Women who are obese having BMI greater than 30 are more susceptible to the threat of Hypovitaminosis D. This is because adipose tissue retains Vitamin D which makes it difficult to circulate in the blood. Vitamin D might help reduce weight gain as it works as a suppressant for appetite [44]. VDRs are present on adipocytes. Higher Vitamin D levels with enhanced calcium levels in adipocytes result in a reduction in the breakdown of fats and lipids. Obesity is interlinked with reduced Vitamin D concentrations and higher PTH concentrations. Lower Vitamin D levels lead to higher levels of parathyroid hormone which leads to an increase in body fat mass and subsequently leads to the formation of fatty acids and triglycerides. Body fat mass is negatively correlated with Vitamin D proportions [45]. An RCT proposed that the women who are supplemented with Vitamin D have more fat loss as compared with the women who deficient [46].
Osteoporosis and Muscle Weakness: Vitamin D helps to form strong bones by utilizing calcium and phosphorus and maintaining the metabolism of bone. Inadequate levels of Vitamin D can cause bone loss, reduction in bone density, osteopenia, osteoporosis & a greater incidence of fractures. Due to the decline in bone density, the prevalence of fractures increases as the bones start to lose calcium [47]. A high proportion of Vitamin D increases muscle performance and decreases muscle weakness and the extent of falls. Patients suffer from weakness and pain in the bones. Hypovitaminosis D affects children with a bone-weakening disease called rickets and it softens the bones in adults called Osteomalacia. Children suffering from rickets have skeletal defects such as bent posture and bent legs [48-50]. It is noteworthy, that rickets can be prevented if the Vitamin D intake is increased and Osteoporotic fractures can be treated. Low Vitamin D levels and severity of bone pain in the legs, joints, and ribs are correlated. Back pain is found to be the most prevalent in women, which indicates the deficiency of Vitamin D among women. A study of around 9000 elderly women, suggested the correlation between reduced serum Vitamin D levels and back pain [51]. In a study, the elderly persons who were given Vitamin D (700 IU/day-800 IU/day), showed a 23%-43% decline in the incidence of hip and non-vertebral fractures.
In another trial, in which the elderly women in Nursing home were given Vitamin D2 and calcium-800 IU/day for five months and 72% decline is found in the incidence of falls In a study of around 1100 menopausal and postmenopausal women of middle age had inadequate levels of Vitamin D suffered from low bone mineral density [52].
The Economic Aspects of Osteoporosis and Osteoarthritis (ESCEO) revealed that in postmenopausal and elderly women, higher intake of Vitamin D levels with sun exposure and supplements can reduce osteoporosis and pain in bones. By increasing the Vitamin D levels in patients having reduced serum Vitamin D, showed fewer symptoms [53].
Fibromyalgia is characterized by the presence of pain in muscles and other areas such as the neck, elbows, knees, chest, and shoulders, associated with other disorders such as fatigue, sleep disorder, and frequent mood changes. It is 9-fold more prevalent in women than men. Progesterone has a major effect on a female’s metabolism and leads to respiratory alkalosis due to the increase in respiration and subsequently, the kidney begins to produce alkaline urine. The association of chronic migraine and Fibromyalgia can be observed in females with lower serum Vitamin D concentration [54]. Low levels of Vitamin D can be a responsible factor for this disorder. Vitamin D2 supplementation or calciferol can help reduce the symptoms.
In a study conducted in Saudi Arabia, in which one hundred women affected with Fibromyalgia were enrolled, they were found to have reduced serum 25(OH)D concentrations. When supplemented with calciferol or Vitamin D2, they showed a reduction in symptoms of fibromyalgia, which suggests the significance of Vitamin D levels in controlling the disorder [55,56].
Multiple sclerosis: In multiple sclerosis, the brain is damaged by its immune cells. Generally, women are found to be more linked with this autoimmune disorder as low serum 25-hydroxyl vitamin concentrations are found in the body. Individuals living at higher latitudes or a distance from the equator are found to be more prone to Multiple sclerosis [57,58]. Additional intake can help to treat multiple sclerosis. In a study of Finnish females, inadequate serum 25(OH) D concentrations lead 43% greater incidence of multiple sclerosis [27]. In a study, approx. 187,000 women were enrolled who consumed 400 IU/day of Vitamin D, 41% decline was observed in the risk of developing multiple sclerosis. Increased consumption of Vit D -280,000 IU/week for 6 weeks can be effective in declining the symptoms of MS in patients [59,60].
Cancer: Sunshine can help to decline the incidence of cancer; however, its role is also related to skin cancer. Vitamin D controls the development of a cell due to the possession of VDRs. If levels of Vitamin D are increased, the cancer rates can come to decline or decreases. Various studies prove the importance of the enhancement of Vitamin D in the inhibition of breast, colon, and prostate cancers. Vitamin D is involved in the maturation of normal cells, stimulates the death of the cancerous/abnormal cell, and prevents the process of angiogenesis-in which new blood vessels are formed to transport O2 and other nutrients for the growth and development of the cell. Mortality rates can be reduced due to cancer if Vitamin D levels are enhanced as it works as an anti-inflammatory agent that helps in reducing the pain severity in cancer patients and it is found that breast and colon cancer rates come to decline by 50% if serum 25-HydroxyVitamin D levels are greater than 32 ng/ml [61]. It is also observed that the women supplemented with similar doses of Vitamin D i.e. 400 IU/day and ‘Ca’-1000 mg/daily for 7 years. The women who had a higher level of Vitamin D-above 24 ng/ml were found to have a 253% reduced risk of colorectal cancer than the women who had lower levels of Vitamin D i.e. <12 ng/ml [30]. In another Randomized-controlled trial in which postmenopausal women who took Vitamin D-1100 IU/day and Ca-1500 mg/day for 4 years found to have a decline in all types of cancers by 60%.
Rheumatoid Arthritis (RA): Studies reveal that lower Vitamin D levels are related to the risk of developing Rheumatoid arthritis. A study conducted for 29,368 women of age 55-69 years revealed that women having low Vitamin D levels were found to suffer from this autoimmune disease. And women having increased Vitamin D concentrations have less possibility for developing RA [62]. It can be prevented with enhanced Vitamin D levels as Vitamin D exhibits the immunomodulation effect and helps in controlling immune responses [63].
Type 1 and Type 2 Diabetes Mellitus: Type1 Diabetes Mellitus (T1DM), an autoimmune disorder in which β-cells of the pancreas are damaged by the immune system, so insulin can’t be formed completely or the body becomes deficient in insulin. Around 1 in 300 children in the United States and 2%-5% globally, it is found to be highly prevalent [64]. Vitamin D serves anti-inflammatory and immunomodulation effect and helps in controlling the secretion of insulin, the existence of beta cells, and maintains the levels of calcium inside the beta cells of the pancreas [65]. It has been shown by various researches that Type I diabetes is linked with Vitamin D deficiency however, can be prevented if Vitamin D fortified milk is supplemented to children. It helps to maintain insulin stimulated by glucose. In a study, newly diagnosed patients were supplemented with different forms of Vitamin D. Alfa-Calcidiol was found to be effective in patients with T1DM whereas other forms of Vitamin D such as cholecalciferol and calcitriol were found to be less effective [34]. It is observed that if offspring are supplemented with Vitamin D during the period of pregnancy, can come out to be beneficial in preventing the development of T1DM by 63% [66].
In Type 2 Diabetes, insulin is not used appropriately by the body which leads to the elevation of sugar in the blood. Vitamin D helps in absorbing calcium which in turn regulates the levels of sugar in the blood. Various studies show that inadequate levels can lead to an individual prone to develop T2DM, however, the use of Vitamin D can be advantageous in maintaining blood sugar levels and insulin resistance [67,68]. A study of 83,779 women having no medical history of diabetes, were divided into 2 groups. They were provided with additional Vitamin D supplementation. In the first group, women were provided with calcium greater than 1200 mg and Vitamin D greater than 800 IU whereas the other group was provided with calcium less than 600 mg and Vitamin D less than 400 IU for about 2-4 years. The first group which is supplemented with higher dosages is found to have a 33% decline in the incidence of Type II diabetes [68-71].
Tuberculosis (TB): In one of the study it was found that in female Tuberculosis patients, factors including poor nutrition, low socioeconomic level, and less exposure to sunlight reflecting deficiency of Vitamin D may increase the possibilities of disease progression. Higher intake of Vitamin D can help to reduce the risk of TB. In the era of without antibiotics, Sunshine and Vitamin D containing food proved as an effective measure in controlling TB [72-74].
Systemic Lupus Erythematous (SLE): SLE can damage various organs and is responsible for inflammation. In this autoimmune disorder, individuals sensitive to sunlight are affected with red-colored rashes on their skin. So, they are advised to get less sun exposure which in turn, will become them Vitamin D deficient. Usually, inadequate levels are found in SLE patients. Vitamin D maintains the development and production of the immune cells involved in SLE.
The immune system can be affected by the deficiency of Vitamin D. Vitamin D has an action of immunomodulation and suppresses many functions of the immune system in individuals with SLE [75]. Higher intake of Vitamin D can show improvements in SLE patients.
Autoimmune Thyroid Disorders (AITD): AITD includes Grave’s diseases and Hashimoto thyroiditis, both are linked to poor Vitamin D intake levels which are associated with reduced serum 25-OHD concentrations. In Grave’s disease, the thyroid gland is damaged by the immune cells of the body which leads to more production of thyroid hormone than is required by the body [76,77]. VDRs are present on many immune cells which regulate the immune system by influencing the immune and adaptive responses. Along with the anti-thyroid drugs or by increasing the thyroid hormone, the use of Vitamin D has been beginning to use as a therapy to combat AITD [78].
Cognitive Disorders: Vitamin D serves a significant function in the maturation and maintenance of the brain and its functions and protection of neurons because its receptors are present in the brain. It is a neuro-steroid hormone, has a significant effect on neurons [79]. Hypovitaminosis D can lead to individuals suffering from Parkinson’s disease, Alzheimer’s disease, schizophrenia, depression, anxiety disorders, and dementia. Vitamin D maintains the functions of neurotransmitters in the brain such as acetylcholine, serotonin, and dopamine. It also acts as an antioxidant agent, has a defensive action on brain from various free radicals.
Vitamin D supplementation proved to be an effective approach to treat cognitive disorders. It is reported in a study that when 800 IU/day Vitamin D was supplemented to individuals affected by Alzheimer’s disease, it is found to be reduced by 5 times after seven years of supplementation. A meta-analysis stated that there is about 2.4 times increased possibility in the insufficient Vitamin D individuals, to think and take decisions properly due to the mental disability as compared with sufficient individuals. Vitamin D supplementation can be done to treat these neural diseases. In a study, in which 170 women of age between 65-77 years were enrolled and after Vitamin D supplementation for some time, it is found that increasing intake of Vitamin D resulted to be beneficial in declining cognitive disorders.
Depression affects the individual’s mood in which he/she has a feeling of sadness and loneliness and begins to withdraw from society and other social activities. Depressive patients tend to go less outside thus, they get less sun exposure and their appetite is generally poor. It is highly prevalent in women. It has been stated in studies that women are at two time’s greater risk to affect with depression than men. Around 840 million individuals suffer from depression worldwide. Lower levels of Vitamin D are responsible for affecting 8%-14% greater risk of depression and 50% greater risk of suicide. Patients who suffer from depression are found to have low serum Vitamin D levels. It is also stated in some studies that individuals who have limited exposure to sunlight, are found to suffer from depression. Harbolic stated in a study in which about 6000 individuals of age around 50 years were enrolled, proposed that individuals suffering from Hypovitaminosis D are more susceptible to suffer from depression (feeling of sadness and loneliness. Sufferers who are getting antidepressants along with Vitamin D are found to help lower depression. Vitamin D performs the function of an anti-inflammatory agent and maintains the production of serotonin in controlling depression [80]. In another study, in which 18 years of adults are enrolled as participants reported to suffer from depression were found to be affected with Hypovitaminosis D. In a study, in which 20 women complained about anxiety disorders such as any kind of fear, responses towards stress or any panic situation, found to have lower serum 25-OHD concentrations. High intake of Vitamin D supplementation by sun exposure and dietary sources can be an effective method to reduce anxiety. In a study of 743 Australian pregnant females having low serum Vit D levels, the infants born were affected with language impairment function.
Cardio Vascular Diseases (CVDs): Vitamin D receptors are present in the heart. Vitamin D maintains the functions of immune and inflammatory cells. Inadequate Vitamin D proportions result in hypertension, Hyperlipidemia, peripheral vascular diseases, coronary artery diseases, heart failure, and stroke [81]. Vitamin D shows an anti-inflammatory effect. Reduced levels can cause inflammation in the arteries. Vitamin D deficiency is also correlated with Atherosclerosis. Vitamin D helps in the regulation of high blood pressure by keeping the arteries flexible and relaxed. High Blood pressure can also be decreased if an individual is supplemented with Vitamin D. In a study, 148 Vit D deficient elderly females were given Vitamin D (800 IU) and calcium (1200 mg), there is 9% decline is found in systolic BP in comparison to calcium alone [82].
Inflammation: Vitamin D serves a significant purpose in maintaining innate and adaptive immune responses. It helps the immune system to synthesize antimicrobial proteins which fight against the bacteria and coping the infections and inflammation. A diet enriched with Vitamin D can help control pain. Vitamin D shows its anti-inflammatory property. It helps to heal wounds by inhibiting inflammation and initiating immune responses in the body. It inhibits the secretion of cytokines and suppresses the function of T-cell [83]. Increased levels of Vitamin D help in lowering inflammation and pain. Vitamin D deficient individuals are found to have a higher level of C-reactive protein which is the marker of inflammation, produced by the liver.
Inflammatory Bowel Disease (IBD): IBD is highly prevalent in Vitamin D deficient individuals. It includes two diseases as Crohn’s disease and ulcerative colitis. Crohn’s disease cause damage to the GI tract and causes diarrhea, pain in the abdomen, fever, and fatigue while ulcerative colitis causes inflammation in the Colon. Although Crohn’s disease is not treatable it can be maintained or reduced with Vitamin D supplementation by sun exposure and dietary intake. In Nurse’s Health studies in the USA, it was observed that women of age around thirty years living at northern latitudes were found to be more prevalent to IBD than women living at southern latitudes. It might be due to easy accessibility of the sun exposure at southern latitudes. Patients supplemented with Vitamin D were found to have a reduction in C-reactive protein (an indicator of inflammation) and fecal calprotectin (a marker of intestinal inflammation). Vitamin D can act as a regulator in the immune system to control inflammation therefore, can be used as a therapy to curb IBD [84].
Fatigue, Tiredness, and Sleep Disorders: Low levels of Vitamin D can cause fatigue. In a case study, it was found that a female having a Vitamin D level of only 5.9 ng/ml, which is considered deficient, suffered from chronic daytime fatigue and headaches. When Vitamin D levels were raised to 39 ng/ml, she started to show reduced symptoms. Therefore, Vitamin D supplementation has been shown to decrease fatigue and tiredness. The association of low levels of Vitamin D and muscle pain and weakness subsequently leads to sleep disturbances. Hypovitaminosis D can cause sleep apnea-a kind of sleep disorder. Insufficient levels of Vitamin D can also make an individual sleep in the daytime by influencing the central inflammatory mediators. Vitamin D regulates many metabolic processes and disruption in sleep can be occurred if any of the metabolic processes is not regulated properly in the absence of Vitamin D [85].
Hair loss: Hair loss mostly occurs due to stress. But low Vitamin D levels can lead to excessive hair loss. It is quite common in women. Vitamin D deficiency can cause Alopecia areata-autoimmune disorder makes severe hair loss on the scalp. Female Pattern Hair Loss (FPHL) is majorly responsible for Alopecia areata in women. The studies suggest that it affects around 6%-12% of females aged between 20-30 years and around 55% of elderly women of age about 70 years. It can be observed in women with low levels of Androgen. Vitamin D supplementation can be useful to reduce hair loss and promote the growth of hair. Sunlight exposure, the use of calcipotriol, and Vitamin D supplements were found to be effective to combat FPHL [86]. Vitamin D receptors are present on keratinocytes, regulates the production of keratin. Keratinocytes can be obtained from hair follicles, which aids the hair follicles to regenerate. FPHL is regulated by estrogen and androgens.
Mortality: It is described in many studies that lower serum Vitamin D concentration can lead to more all-cause mortality cases. But the increased Vitamin D concentrations in patients can lead to a lower incidence of mortality cases by 4%-11% [20]. Supplementation with Vitamin D3 was found to be more effective than Vitamin D2 in reducing deaths. However, increased intake can also lead to death due to Hypervitaminosis D. In a meta-analysis in which mostly elderly women were enrolled of age around 70 years, it showed that there is a decline in mortality rates by 7% by increasing the Vitamin D intake [87].
Uterine Fibroids (UF): It affects the reproductive tract of women. These benign tumors affect around 77% of women. It is found to be four times more prevalent in females with dark pigmentation than light-skin pigmentation because of Vitamin D deficiency. It can further have associated with miscarriage, pelvic pain, heavy and painful menstruation. VDRs are present in the uterus and help in the regulation of the menstrual cycle and the gene expression which influences the maintenance of uterine tissues. Vitamin D therapy can be used in which it serves the function of antifibrotic property and can help in the reduction in the number and volume of uterine fibroid lesions by stimulating the death of these tumors. Patients having UF lesions were found to have lower Vitamin D levels [88].
Anemia: Anemia is a major issue, affects majorly children and women. Vitamin D is involved in the regulation of iron levels in the body as well as the formation of RBCs. It maintains the levels of cytokines involving in inflammation and the production of antimicrobial peptides. It decreases the ‘hepcidin’ hormone during inflammation which is responsible for maintaining iron levels in the body. Vitamin D deficiency disrupts the regulation which ultimately leads to iron loss and the individual can become anemic. Patients with inadequate serum 25(OH)D concentrations are more prone to anemia. Higher levels of Vitamin D can elevate the number of RBC and hemoglobin levels [89].
Polycystic Ovary Syndrome (PCOS): PCOS affects the regulation of the menstruation cycle. It leads to elevated androgen hormones in the women’s body and leads to irregular menstruation. As the VDRs are present on the ovary, it is involved in the maintenance of functions of ovary. Obese PCOS patients were found to have lower serum 25-(OH) D concentrations than non-obese patients [90]. Higher consumption of Vitamin D can be effective in the proper growth of ovarian follicles and the regulation of the menstrual cycle.
Infection and Covid-19: Recent researches suggest that individuals who are deficient in Vitamin D levels have a greater possibility to become infected with the COVID-19 virus. Globally, the COVID-19 has made health issues and affecting the respiratory tract. Many studies demonstrated that Vitamin D plays a very important role in preventing respiratory tract disorder. In human lung microvascular endothelial cells, Vitamin D increases the number of the ACE2 receptors which can attach to the virus and inactivate the virus. It has been found that in reducing the common cold, Vitamin D can increase cellular immunity, physical immunity and regulate adaptive immunity pathways. Hence people who are deficient or at high risk of Vitamin D should include Vitamin D supplements or fortified food in their diet during the COVID-19 pandemic [91,92].
Vitamin D helps us to make our immune system strong. Vitamin D deficiency can cause infection in the upper respiratory tract. In a study, of 2279 children, children having low Vitamin D levels, were affected by lower respiratory tract infections. Increased levels of Vitamin D can help reduce the infections such as flu, colds, bronchitis, wheezing disorders, pneumonia, bacteremia, and urinary tract infections. Deficient children suffer more from wheezing disorders. Flu and the common cold are found to be more prevalent in colder months when Vitamin D levels are found to be low in individuals. High intake of Vitamin D leads to an increase in the formation of anti-microbial proteins which helps to fight against pathogens-viruses and bacteria. High Vitamin D levels also reduce the incidence of asthma and allergies [93]. A study among the Japanese children supplemented with 1200 IU/day of Vitamin D was found to be reduced by 42% in Influenza. According to study children with higher Vitamin D level have 93% less risk of infections than Vitamin D deficient children [94].
Along with high Vitamin D intake, maintaining distance with people and personal hygiene are found to be effective in combating COVID-19 infection.
Conclusion
Vitamin D is important for optimal skeletal and bone health. Vitamin D is also considered to be associated with many chronic disorders. Besides play important role in the prevention of various disorders includes diabetes, rheumatoid, osteoporosis, and hypertension, reduced risk of cancer, autoimmune disorder, and extraskeletal disease. With increasing urbanization and changing, lifestyles people are less exposed to sunlight which affects human health. Hence changing the dietary pattern includes Vitamin D fortified food or supplements may enhance the Vitamin D concentration. Considering fortification of varieties of staple food may be the effective solution to overcome Vitamin D deficiency not only in the high but low-income group.
Declarations
Conflicts of Interest
The authors declared no potential conflicts of interest concerning the research, authorship, and/or publication of this article.
References
- Belsey, Richard, et al. "The physiologic significance of plasma transport of vitamin D and metabolites." The American Journal of Medicine, Vol. 57, No. 1, 1974, pp. 50-56.
- Haddad, John G., and Kyung Ja Chyu. "Competitive protein-binding radioassay for 25-hydroxycholecalciferol." The Journal of Clinical Endocrinology & Metabolism, Vol. 33, No. 6, 1971, pp. 992-95.
- Chen, Tai C., Adrian K. Turner, and Michael F. Holick. "Methods for the determination of the circulating concentration of 25-hydroxyvitamin D." Journal of Nutritional Biochemistry, Vol. 1, No. 6, 1990, pp. 315-19.
- Dawson-Hughes, Bess, et al. "Estimates of optimal vitamin D status." Osteoporosis International, Vol. 16, 2005, pp. 713-16.
- SACN Update on Vitamin D-2007 The Scientific Advisory Committee on Nutrition update on current evidence on Vitamin D. https://www.gov.uk/government/publications/sacn-update-on-vitamin-d-2007
- Samefors, Maria, et al. "Vitamin D deficiency in elderly people in Swedish nursing homes is associated with increased mortality." European Journal of Endocrinology, Vol. 170, No. 5, 2014, pp. 667-75.
- Cancer Research UK. "Vitamin D expert review." 2010. https://www.nice.org.uk/guidance/ph32/documents/expert-paper-3-vitamin-d2
- Thacher, Tom D., and Bart L. Clarke. "Vitamin D insufficiency." Mayo Clinic Proceedings, Vol. 86, No. 1, 2011, pp. 50-60.
- Yosephin, Betty, et al. "Food sources of vitamin D and its deficiency in worker women." ASEAN/Asian Academic Society International Conference Proceeding Series, 2016.
- McCance, R. A., and E. M. Widdowson. "The Composition of Foods, 6th summary edn." Compiled by the Food Standards Agency and Institute of Food Research: UK, 2002.
- Department of Health (DoH). "Dietary reference values for food energy and nutrients for the United Kingdom." London: Her Majesty's Stationery Office (HMSO), 1991.
- Holick, Michael F., et al. "Evaluation, treatment, and prevention of vitamin D deficiency: An Endocrine Society clinical practice guideline." The Journal of Clinical Endocrinology & Metabolism, Vol. 96, No. 7, 2011, pp. 1911-30.
- Holick, Michael F. "Sunlight and vitamin D for bone health and prevention of autoimmune diseases, cancers, and cardiovascular disease." The American Journal of Clinical Nutrition, Vol. 80, No. 6, 2004, pp. 1678S-88S.
- Kauffman, Joel M. "Benefits of vitamin D supplementation." Journal of American Physicians and Surgeons, Vol. 14, No. 2, 2009, pp. 38-45.
- Bar, A., et al. "Performance and bone development in broiler chickens given 25-hydroxycholecalciferol." British Poultry Science, Vol. 44, No. 2, 2003, pp. 224-33.
- Boris, A., et al. "Structure-activity relationships of compounds related to vitamin D." Endocrinology of Calcium Metabolism/Editor, JA Parsons, 1982, pp. 297-320.
- Bouillon, Roger, P. V. Kerkhove, and Pieter De Moor. "Measurement of 25-hydroxyvitamin D3 in serum." Clinical Chemistry, Vol. 22, No. 3, 1976, pp. 364-68.
- Cantor, A., and W. Bacon. "Performance of caged broilers fed vitamin D3 and 25-(OH) vitamin D3." Poultry Science, Vol. 57, 1978, pp. 1123-24.
- Chen Jr, Philip S., and H. Bruce Bosmann. "Effect of vitamins D2 and D3 on serum calcium and phosphorus in rachitic chicks." The Journal of Nutrition, Vol. 83, No. 2, 1964, pp. 133-39.
- DeLuca, Hector F. "Overview of general physiologic features and functions of vitamin D." The American Journal of Clinical Nutrition, Vol. 80, No. 6, 2004, pp. 1689S-96S.
- Driver, J. P., et al. "The effect of maternal dietary vitamin D3 supplementation on performance and tibial dyschondroplasia of broiler chicks." Poultry Science, Vol. 85, No. 1, 2006, pp. 39-47.
- Edwards Jr, Hardy M. "The effect of dietary cholecalciferol, 25-hydroxycholecalciferol and 1, 25-dihydroxycholecalciferol on the development of tibial dyschondroplasia in broiler chickens in the absence and presence of disulfiram." The Journal of Nutrition, Vol. 119, No. 4, 1989, pp. 647-52.
- Zella, Julia B., and Hector F. DeLuca. "Vitamin D and autoimmune diabetes." Journal of Cellular Biochemistry, Vol. 88, No. 2, 2003, pp. 216-22.
- Holick, Michael F. "High prevalence of vitamin D inadequacy and implications for health." Mayo Clinic Proceedings, Vol. 81, No. 3, 2006, pp. 353-73.
- Santorelli, Gillian, et al. "Associations of maternal vitamin D, PTH and calcium with hypertensive disorders of pregnancy and associated adverse perinatal outcomes: Findings from the Born in Bradford cohort study." Scientific Reports, Vol. 9, No. 1, 2019, pp. 1-9.
- Amegah, A. Kofi, Moses K. Klevor, and Carol L. Wagner. "Maternal vitamin D insufficiency and risk of adverse pregnancy and birth outcomes: A systematic review and meta-analysis of longitudinal studies." PLoS One, Vol. 12, No. 3, 2017, p. e0173605.
- McDonnell, Sharon L., et al. "Maternal 25 (OH) D concentrations = 40 ng/mL associated with 60% lower preterm birth risk among general obstetrical patients at an urban medical center." PloS One, Vol. 12, No. 7, 2017, p. e0180483.
- Qin, Lu-Lu, et al. "Does maternal vitamin D deficiency increase the risk of preterm birth: A meta-analysis of observational studies." Nutrients, Vol. 8, No. 5, 2016, p. 301.
- Tabatabaei, Negar, et al. "Maternal vitamin D insufficiency early in pregnancy is associated with increased risk of preterm birth in ethnic minority women in Canada." The Journal of Nutrition, Vol. 147, No. 6, 2017, pp. 1145-51.
- Roth, Daniel E., et al. "Vitamin D supplementation during pregnancy: State of the evidence from a systematic review of randomised trials." BMJ, Vol. 359, 2017, p. j5237.
- Ross, A. Catharine, et al. "Committee to Review Dietary Reference Intakes for Vitamin D and Calcium, Institute of Medicine. Dietary reference intakes for calcium and vitamin D." National Academy Press, Washington, DC, 2011.
- Zhang, Runhua, et al. "Serum 25-hydroxyvitamin D and the risk of cardiovascular disease: Dose-response meta-analysis of prospective studies." The American Journal of Clinical Nutrition, Vol. 105, No. 4, 2017, pp. 810-19.
- Ibrahim, Mohanad Kamaleldin Mahmoud, and Mustafa Khidir Mustafa Elnimeiri. "Non-classical presentation of vitamin D deficiency: a case report." Journal of Medical Case Reports, Vol. 14, No. 1, 2020, pp. 1-3.
- Chisty, Syed Javed S., and Diganta Das. "Vitamin D in pregnancy-an overview." Journal of Obstetrics & Gynaecology Barpeta, Vol. 1, No.1, 2014, pp. 17-23.
- Mannion, Cynthia A., Katherine Gray-Donald, and Kristine G. Koski. "Association of low intake of milk and vitamin D during pregnancy with decreased birth weight." CMAJ, Vol. 174, No. 9, 2006, pp. 1273-77.
- Weiss, S. T., and A. A. Litonjua. "Childhood asthma is a fat-soluble vitamin deficiency disease." Clinical & Experimental Allergy, Vol. 38, No. 3, 2008, pp. 385-87.
- Wang, Hanmin, et al. "Vitamin D and chronic diseases." Aging and Disease, Vol. 8, No. 3, 2017, pp. 346-53.
- Givens, Maurice H., and Icie G. Macy. "The chemical composition of the human fetus." Journal of Biological Chemistry, Vol. 102, No. 1, 1933, pp. 7-17.
- Trotter, Mildred, and Barbara B. Hixon. "Sequential changes in weight, density, and percentage ash weight of human skeletons from an early fetal period through old age." The Anatomical Record, Vol. 179, No. 1, 1974, pp. 1-18.
- Kovacs, Christopher S., and Henry M. Kronenberg. "Maternal-fetal calcium and bone metabolism during pregnancy, puerperium, and lactation." Endocrine Reviews, Vol. 18, No. 6, 1997, pp. 832-72.
- Kovacs, Christopher S. "Calcium and bone metabolism in pregnancy and lactation." The Journal of Clinical Endocrinology & Metabolism, Vol. 86, No. 6, 2001, pp. 2344-48.
- Del Valle, Heather B., et al., eds. "Dietary reference intakes for calcium and vitamin D." 2011.
- Bischoff-Ferrari, Heike A., et al. "Higher 25-hydroxyvitamin D concentrations are associated with better lower-extremity function in both active and inactive persons aged= 60 y." The American Journal of Clinical Nutrition, Vol. 80, No. 3, 2004, pp. 752-58.
- Bischoff-Ferrari, Heike A., et al. "Effect of vitamin D on falls: A meta-analysis." JAMA, Vol. 291, No. 16, 2004, pp. 1999-2006.
- Cantorna, Margherita T., et al. "Vitamin D status, 1, 25-dihydroxyvitamin D3, and the immune system." The American Journal of Clinical Nutrition, Vol. 80, No. 6, 2004, pp. 1717S-20S.
- Abdali, Daniyal, Sue E. Samson, and Ashok Kumar Grover. "How effective are antioxidant supplements in obesity and diabetes?" Medical Principles and Practice, Vol. 24, No. 3, 2015, pp. 201-15.
- Wintermeyer, Elke, et al. "Crucial role of vitamin D in the musculoskeletal system." Nutrients, Vol. 8, No. 6, 2016, p. 319.
- Wacker, Matthias, and Michael F. Holick. "Vitamin D-effects on skeletal and extraskeletal health and the need for supplementation." Nutrients, Vol. 5, No. 1, 2013, pp. 111-48.
- Knutsen, Kirsten Valebjørg, et al. "Vitamin D status in patients with musculoskeletal pain, fatigue and headache: A cross-sectional descriptive study in a multi-ethnic general practice in Norway." Scandinavian Journal of Primary Health Care, Vol. 28, No. 3, 2010, pp. 166-71.
- Winzenberg, Tania, et al. "Vitamin D: And the musculoskeletal health of older adults." Australian Family Physician, Vol. 41, No. 3, 2012, pp. 92-99.
- Adams, John S., and Gene Lee. "Gains in bone mineral density with resolution of vitamin D intoxication." Annals of Internal Medicine, Vol. 127, No. 3, 1997, pp. 203-06.
- Anglin, Rebecca ES, et al. "Vitamin D deficiency and depression in adults: Systematic review and meta-analysis." The British Journal of Psychiatry, Vol. 202, No. 2, 2013, pp. 100-07.
- Spedding, Simon. "Vitamin D and depression: A systematic review and meta-analysis comparing studies with and without biological flaws." Nutrients, Vol. 6, No. 4, 2014, pp. 1501-18.
- Natasja, M., and P. Lips. "Worldwide vitamin D status." Best Practice & Research. Clinical Endocrinology & Metabolism, Vol. 25, No. 4, 2011, pp. 671-80.
- Ardawi, M-SM, et al. "High prevalence of vitamin D deficiency among healthy Saudi Arabian men: Relationship to bone mineral density, parathyroid hormone, bone turnover markers, and lifestyle factors." Osteoporosis International, Vol. 23, No. 2, 2012, pp. 675-86.
- Alharbi, Fatimah M. "Update in vitamin D and multiple sclerosis." Neurosciences, Vol. 20, No. 4, 2015, pp. 329-35.
- Hanwell, Heather EC, and Brenda Banwell. "Assessment of evidence for a protective role of vitamin D in multiple sclerosis." Biochimica et Biophysica Acta (BBA)-Molecular Basis of Disease, Vol. 1812, No. 2, 2011, pp. 202-12.
- Schwarz, Stefan, and Hans Leweling. "Multiple sclerosis and nutrition." Multiple Sclerosis Journal, Vol. 11, No. 1, 2005, pp. 24-32.
- Chaudhuri, Abhijit. "Why we should offer routine vitamin D supplementation in pregnancy and childhood to prevent multiple sclerosis." Medical Hypotheses, Vol. 64, No. 3, 2005, pp. 608-18.
- Cantorna, Margherita T. "Vitamin D and its role in immunology: Multiple sclerosis, and inflammatory bowel disease." Progress in Biophysics and Molecular Biology, Vol. 92, No. 1, 2006, pp. 60-64.
- Holick, Michael F. "Vitamin D: Importance in the prevention of cancers, type 1 diabetes, heart disease, and osteoporosis." The American Journal of Clinical Nutrition, Vol. 79, No. 3, 2004, pp. 362-71.
- Kostoglou-Athanassiou, Ifigenia, et al. "Vitamin D and rheumatoid arthritis." Therapeutic Advances in Endocrinology and Metabolism, Vol. 3, No. 6, 2012, pp. 181-87.
- Baker, Joshua F., et al. "Associations between vitamin D, disease activity, and clinical response to therapy in rheumatoid arthritis." Clinical and Experimental Rheumatology-Incl Supplements, Vol. 30, No. 5, 2012, pp. 658-64.
- Vaisberg, Mauro W., et al. "Influence of cholecalciferol (vitamin D3) on the course of experimental systemic lupus erythematosus in F1 (NZBxW) mice." Journal of Clinical Laboratory Analysis, Vol. 14, No. 3, 2000, pp. 91-96.
- Merlino, Linda A., et al. "Vitamin D intake is inversely associated with rheumatoid arthritis: Results from the Iowa Women's Health Study." Arthritis & Rheumatism: Official Journal of the American College of Rheumatology, Vol. 50, No. 1, 2004, pp. 72-77.
- Jankosky, Christopher, et al. "Viruses and vitamin D in the etiology of type 1 diabetes mellitus and multiple sclerosis." Virus Research, Vol. 163, No. 2, 2012, pp. 424-30.
- Nikooyeh, Bahareh, et al. "Daily consumption of vitamin D-or vitamin D+ calcium-fortified yogurt drink improved glycemic control in patients with type 2 diabetes: A randomized clinical trial." The American Journal of Clinical Nutrition, Vol. 93, No. 4, 2011, pp. 764-71.
- Gagnon, Claudia, et al. "Serum 25-hydroxyvitamin D, calcium intake, and risk of type 2 diabetes after 5 years: Results from a national, population-based prospective study (the Australian Diabetes, Obesity and Lifestyle study)." Diabetes Care, Vol. 34, No. 5, 2011, pp. 1133-38.
- Menon, Ravi K., et al. "The effects of vitamin D 2 or D 3 supplementation on glycaemic control and related metabolic parameters in people at risk of type 2 diabetes: Protocol of a randomised double-blind placebo-controlled trial." BMC Public Health, Vol. 13, No. 1, 2013, pp. 1-11.
- Brown, Edward M., et al. "Cloning and characterization of an extracellular Ca 2+-sensing receptor from bovine parathyroid." Nature, Vol. 366, No. 6455, 1993, pp. 575-80.
- Vieth, Reinhold. "The pharmacology of vitamin D, including fortification strategies." Vitamin D 2, 2005, pp. 995-1015.
- Talat, Najeeha, et al. "Vitamin D deficiency and tuberculosis progression." Emerging Infectious Diseases, Vol. 16, No. 5, 2010, pp. 853-55.
- Wejse, Christian, et al. "Vitamin D as supplementary treatment for tuberculosis: A double-blind, randomized, placebo-controlled trial." American Journal of Respiratory and Critical Care Medicine, Vol. 179, No. 9, 2009, pp. 843-50.
- Nnoaham, Kelechi E., and Aileen Clarke. "Low serum vitamin D levels and tuberculosis: A systematic review and meta-analysis." International Journal of Epidemiology, Vol. 37, No. 1, 2008, pp. 113-19.
- Hassanalilou, Tohid, et al. "Role of vitamin D deficiency in systemic lupus erythematosus incidence and aggravation." Autoimmunity Highlights, Vol. 9, No. 1, 2018, p. 1.
- Mackawy, Amal Mohammed Husein, Bushra Mohammed Al-Ayed, and Bashayer Mater Al-Rashidi. "Vitamin D deficiency and its association with thyroid disease." International Journal of Health Sciences, Vol. 7, No. 3, 2013, pp. 267-75.
- Baeke, Femke, et al. "Vitamin D: Modulator of the immune system." Current Opinion in Pharmacology, Vol. 10, No. 4, 2010, pp. 482-96.
- Tamer, Gonca, et al. "Relative vitamin D insufficiency in Hashimoto's thyroiditis." Thyroid, Vol. 21, No. 8, 2011, pp. 891-96.
- D Carter, Graham. "Accuracy of 25-hydroxyvitamin D assays: Confronting the issues." Current Drug Targets, Vol. 12, No. 1, 2011, pp. 19-28.
- Slinin, Y., et al. "25-Hydroxyvitamin D levels and cognitive performance and decline in elderly men." Neurology, Vol. 74, No. 1, 2010, pp. 33-41.
- Lavie, Carl J., et al. "Vitamin D and cardiovascular health." Circulation, Vol. 128, No. 22, 2013, pp. 2404-06.
- Norman, P. E., and J. T. Powell. "Vitamin D and cardiovascular disease." Circulation Research, Vol. 114, No. 2, 2014, pp. 379-93.
- Koutkia, Polyxeni, Tai C. Chen, and Michael F. Holick. "Vitamin D intoxication associated with an over-the-counter supplement." New England Journal of Medicine, Vol. 345, No. 1, 2001, pp. 66-67.
- Fletcher, Jane, et al. "The role of vitamin D in inflammatory bowel disease: Mechanism to management." Nutrients, Vol. 11, No. 5, 2019, p. 1019.
- Johnson, Kevin, and Maryam Sattari. "Vitamin D deficiency and fatigue: An unusual presentation." SpringerPlus, Vol. 4, No. 1, 2015, pp. 1-4.
- Almohanna, Hind M., et al. "The role of vitamins and minerals in hair loss: A review." Dermatology and Therapy, Vol. 9, No. 1, 2019, pp. 51-70.
- Melamed, Michal L., et al. "25-hydroxyvitamin D levels and the risk of mortality in the general population." Archives of Internal Medicine, Vol. 168, No. 15, 2008, pp. 1629-37.
- Ciebiera, Michal, et al. "Vitamin D and uterine fibroids-Review of the literature and novel concepts." International Journal of Molecular Sciences, Vol. 19, No. 7, 2018, p. 2051.
- Park, Sook-Hyun. "Maternal Anemia and Vitamin D deficiency: Associations with neonatal hemoglobin levels and the vitamin D status." Perinatology, Vol. 28, No. 1, 2017, pp. 4-10.
- Umar, Meenakshi, et al. "Vitamin D and the pathophysiology of inflammatory skin diseases." Skin Pharmacology and Physiology, Vol. 31, No. 2, 2018, pp. 74-86.
- Zhou, Yun-Fang, Bang-An Luo, and Lu-Lu Qin. "The association between vitamin D deficiency and community-acquired pneumonia: A meta-analysis of observational studies." Medicine, Vol. 98, No. 38, 2019, p. e17252.
- Grant, William B., et al. "Evidence that vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths." Nutrients, Vol. 12, No. 4, 2020, p. 988.
- Bischoff-Ferrari, Heike A., et al. "Benefit-risk assessment of vitamin D supplementation." Osteoporosis International, Vol. 21, No. 7, 2010, pp. 1121-32.
- Charoenngam, Nipith, et al. "The effect of various doses of oral vitamin D3 supplementation on gut microbiota in healthy adults: A randomized, double-blinded, dose-response study." Anticancer Research, Vol. 40, No. 1, 2020, pp. 551-56.