Research - International Journal of Medical Research & Health Sciences ( 2020) Volume 9, Issue 7
Prevalence of Thyroid Dysfunction in Down’s Syndrome
Mandar Ambike1* and Dnyandeo Chopade22Genetic Health and Research Centre, Nashik, India
Mandar Ambike, Symbiosis Medical College for Woman, Symbiosis International (Deemed) University, Lavale,Pune, India, Tel: 91 20 - 61930003, Email: mandar.ambike@smcw.siu.edu.in
Received: 03-Jun-2020 Accepted Date: Jul 22, 2020 ; Published: 29-Jul-2020
Abstract
Introduction: Association of Down’s syndrome and Hypothyroidism is reported since long time. It is difficult to diagnose Hypothyroidism in Down’s syndrome as the symptoms overlap. Different studies reveal different views regarding the association. So in present study we tried to find out the association between Down’ syndrome and Hypothyroidism.
Methodology: Present study was conducted at “Down Syndrome Care Association, Nashik, India”. The study group was 68 known cases of Down’s syndrome. TSH levels were obtained from blood sample at the earliest. Data was analysed statistically.
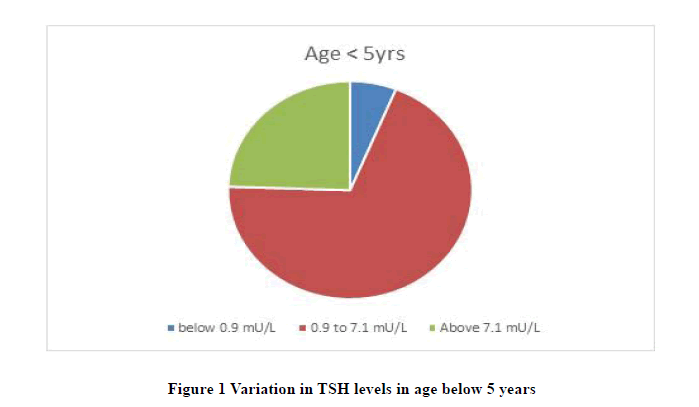
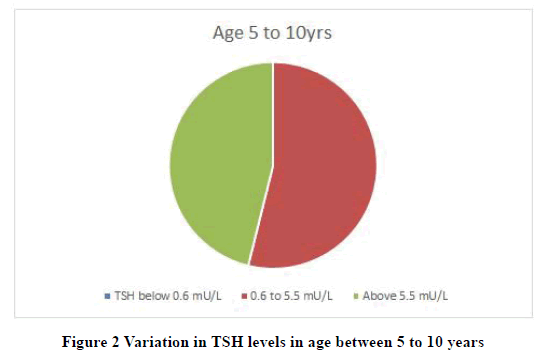
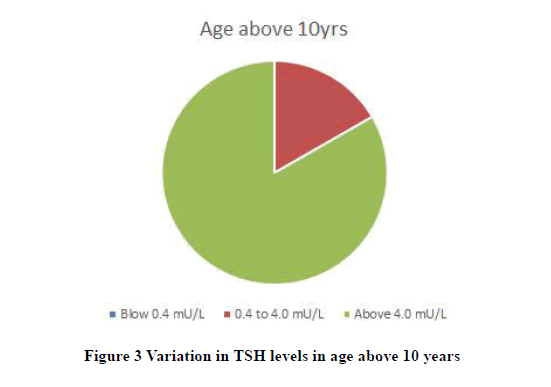
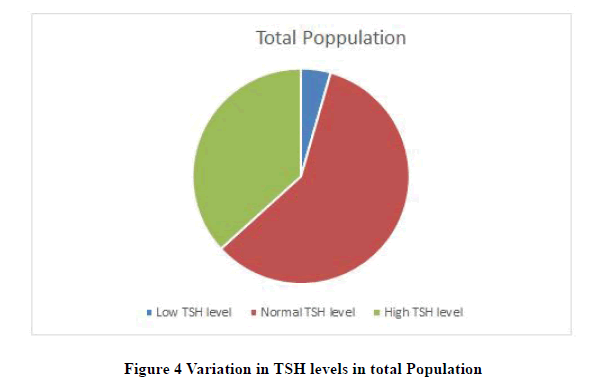
Results: Overall population had 36% cases had high TSH levels. High TSH level in children below 5 years is 24%. The high level of TSH in children of the age group 5 years to 10 years is 46%. And percentage of children above the age of 10 years with high TSH level is 83.34%.
Conclusion: Percentage of thyroid dysfunction is defiantly higher in children’s suffering from Down’ syndrome than normal population. Percentage goes higher as the age increases, so periodic check-up of thyroid function is recommendeds.
Keywords
Down’s syndrome, Thyroid dysfunction, Thyroid stimulating hormone
Introduction
Association of Down’s syndrome and Hypothyroidism was reported since 1866 [1]. Thereafter many studies also reported this association [2,3]. Wide variations were reported regarding the association of Thyroid dysfunction with Down’s syndrome. Thyroid dysfunction in Down’s syndrome adds up to many conditions like developmental delay, cardiopulmonary and gastrointestinal abnormalities [4,5]. The frequency of hypothyroidism was found to be 28 times more in new-born children’s than the normal population [1]. It was also reported that percentage of individuals with Down’s syndrome, the chances of Thyroid dysfunction increase with the age [6]. Studies have shown different views regarding the association as it is difficult to differentiate the symptoms of Downs’s syndrome and Hypothyroidism [1]. Most of the studies recommend regular check-up for thyroid function while few studies think it is not necessary [7]. Present study is attempted to investigate into the association of Thyroid dysfunction and Down’s syndrome in children of increasing age group.
Materials and Methods
This study was conducted at “Down Syndrome Care Association, Nashik, India”. This study was carried out since 2009. The inclusion criteria were all participants in the study should be a proven case of Down’s syndrome. Consent was taken from the parents for the study. The sample size was 68. As the case was diagnosed for Down’s syndrome, the blood samples were collected from each of the cases and tested for levels of Thyroid Stimulating Hormone (TSH). Different age groups were identified and data was segregated. The data was statistically analysed and results were drawn. The findings were compared to the standard TSH level in normal individuals and results were obtained.
Results
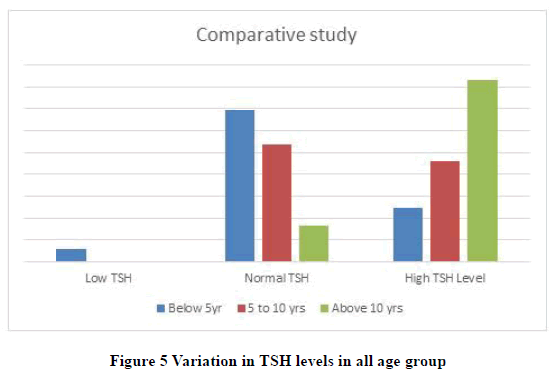
There is a large variation in TSH levels in different age groups. The TSH levels in new-born has a vast range (Average range 0.9 mU/L to 7.1 mU/L). It settles down as age increases. In School going children (age 5 to 10 yrs.) it comes down to 0.6 mU/L to 5.5 mU/L. While it further settles in older age (0.4 mU/L to 4 mU/L). Present study population was divided this in three different groups i.e. Children below the age of 5 yrs, Second group of children from 5 yrs. to 10 yrs, and third group of children above 10 yrs. to 18yrs (Tables 1-5 and Figures 1-5).
| TSH | below 0.9 mU/L | 0.9 to 7.1 mU/L | Above 7.1 mU/L |
|---|---|---|---|
| Age below 5 yrs. | 3 | 34 | 12 |
| (N=49) | 6.12% | 69.38% | 24.50% |
| TSH | TSH below 0.6 mU/L | 0.6 mU/L to 5.5 mU/L | Above 5.5 mU/L |
|---|---|---|---|
| Age 5 to 10 yrs | Nil | 7 | 6 |
| (N=13) | 0% | 53.85% | 46.15% |
| TSH | Blow 0.4 mU/L | 0.4 mU/L to 4.0 mU/L | Above 4.0 mU/L |
|---|---|---|---|
| Age above 10 yrs | Nil | 1 | 5 |
| (N=6) | 0% | 16.66% | 83.34% |
| Total Population | Low TSH level | Normal TSH level | High TSH level |
|---|---|---|---|
| N=68 | 3 | 40 | 25 |
| 4.41% | 58.82% | 36.77% |
| Age | Low TSH | Normal TSH | High TSH Level |
|---|---|---|---|
| Below 5yrs | 6.12% | 69.38% | 24.50% |
| 5 to 10 yrs | 0% | 53.85% | 46.15% |
| Above 10 yrs | 0% | 16.66% | 83.34% |
Discussion
Among all the endocrine disorders Thyroid dysfunction is common in children’s, especially the Hypothyroidism [8- 11]. TSH level is often high in new-borns, which settles down, reflecting altered nature of thyroid axis [4,12-14]. The prevalence of Hypothyroidism in India is around 9% to 11%, which is more than any western country. It is slightly at a higher range in Females [15]. Hypothyroidism in children is associated with impaired physical learning development. So TSH values are important for diagnose and treatment of hypothyroidism. TSH values also help for the monitoring of thyroid replacement therapy [16]. Down’s syndrome (trisomy 21) is again most common genetic disorder (1:800) and most common cause of mental retardation [17,18]. The developmental problems (Physical or Mental) may be mild to severe [19].
The clinical manifestations of Hypothyroidism may be overlapped by Downs’s syndrome [20]. Association of Down’s syndrome with Hypothyroidism is recognised by most of the screening for Hypothyroidism in children’s having Down’s syndrome becomes essential thing. Also periodic monitoring becomes mandatory [21,22], and proper hormone replacement therapy should be administered [23,24].
The result in our study shows overall 36.77% children’s show TSH levels higher than the normal. So it is quite higher than the normal population without Down’s syndrome. Other studies have shown varied percentage. Study performed in Mattel Children’s Hospital, University of California reported 32% more in children suffering from Down’s to normal population [25]. Study carried out at Duke University Medical centre reported 28 times more common with Down’s than normal children’s [26]. One study reported a lifetime prevalence ranging from 13% to 63% [6,27]. While some claim 28% more frequency in neonates and 12% more as age increases 1. Study performed at University of Witwatersrand reported frequency of thyroid dysfunction increase with age 8 years [28]. But some study in Manchester Hospital, UK states that 70% children’s reported normal TSH level in second test so, Hypothyroidism in Down’s syndrome should not be over diagnosed and there is no need of yearly screening up to 20 years [7].
Our study showed results similar to previous studies. Percentage of high TSH level in children below 5 years is 24%. The high level of TSH in children of the age group 5 years to 10 years is 46%. And percentage of children above the age of 10 years with high TSH level is 83.34%. It reveals that overall study group with Down’s syndrome had 36.77 % children’s with high TSH levels. It also reveals that the percentage goes higher as the age increases.
Conclusion
From our study we found the high percentage of children’s suffering from Down’s syndrome is having Thyroid dysfunction (high TSH levels). So Thyroid profile of every child with Down’s syndrome should be done for the early diagnosis and Thyroid dysfunction should be dealt with the proper hormone replacement therapy. Follow-up of Thyroid profile should be kept every year to monitor the changes age wise as well as with the treatment.
Declarations
Conflicts of Interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
References
- Coleman, Mary. "Thyroid dysfunction in down syndrome: A review." Down Syndrome Research and Practice, Vol. 2, No. 3, 1994, pp. 112-5.
- Pascanu, I., et al. "Thyroid dysfunction in children with down's syndrome." Acta Endocrinologica, Vol. 5, No. 1, 2009, pp. 85-92.
- Pierce, Melinda J., Stephen H. LaFranchi, and Joseph D. Pinter. "Characterization of thyroid abnormalities in a large cohort of children with Down syndrome." Hormone Research in Paediatrics, Vol. 87, No. 3, 2017, pp. 170-8.
- Iughetti, Lorenzo, et al. "Thyroid function in Down syndrome." Expert Review of Endocrinology and Metabolism, Vol. 10, No. 5, 2015, pp. 525-32.
- Vigone, Maria Cristina, et al. "Mild hypothyroidism in childhood: Who, when, and how should be treated?" Journal of the Endocrine Society, Vol. 2, No. 9, 2018, pp. 1024-39.
- Fort, P., et al. "Abnormalities of thyroid function in infants with Down syndrome." The Journal of Paediatrics, Vol. 104, No. 4, 1984, pp. 545-49.
- Gibson, P. A., et al. "Longitudinal study of thyroid function in Down’s syndrome in the first two decades." Archives of Disease in Childhood, Vol. 90, No. 6, 2005, pp. 574-8.
- Hong, Hyun Sook, Ji Ye Lee, and Sun Hye Jeong. "Thyroid disease in children and adolescents." Ultrasonography, Vol. 36, No. 4, 2017, p. 289.
- Bettendorf, Markus. "Thyroid disorders in children from birth to adolescence." European Journal of Nuclear Medicine and Molecular Imaging, Vol. 29, No. 2, 2002, pp. S439-446.
- Desai, Meena P. "Thyroid function in children." Journal of the Association of Physicians of India, Vol. 59, 2011, pp. 35-42.
- Singh, Amitabh, et al. "Prevalence of thyroid disorders in children at a tertiary care hospital in western India." Journal of Clinical and Diagnostic Research, Vol. 10, No. 2, 2016, pp. SC01-04.
- Pueschel, Siegfried M., et al. "Thyroid function in Down syndrome." Research in Developmental Disabilities, Vol. 12, No. 3, 1991, pp. 287-96.
- Kaplowitz, Paul B. "Subclinical hypothyroidism in children: Normal variation or sign of a failing thyroid gland?" International Journal of Pediatric Endocrinology, Vol. 2010, No. 1, 2010, pp. 1-8.
- Cutler, Ann T., Rita Benezra-Obeiter, and Stuart J. Brink. "Thyroid function in young children with Down syndrome." American Journal of Diseases of Children, Vol. 140, No. 5, 1986, pp. 479-83.
- Unnikrishnan, Ambika Gopalakrishnan, and Usha V. Menon. "Thyroid disorders in India: An epidemiological perspective." Indian Journal of Endocrinology and Metabolism, Vol. 15, No. 2, 2011, pp. S78-81.
- Kapelari, Klaus, et al. "Pediatric reference intervals for thyroid hormone levels from birth to adulthood: A retrospective study." BMC Endocrine Disorders, Vol. 8, No. 1, 2008, p. 15.
- Karlsson, Bengt, et al. "Thyroid dysfunction in Down’s syndrome: Relation to age and thyroid autoimmunity." Archives of Disease in Childhood, Vol. 79, No. 3, 1998, pp. 242-5.
- Amr, Nermine H. "Thyroid disorders in subjects with Down syndrome: An update." Acta Bio Medica: Atenei Parmensis, Vol. 89, No. 1, 2018, pp. 132-9.
- Smith, Liz. "Updated AAP guidelines on newborn screening and therapy for congenital hypothyroidism." American Family Physician, Vol. 76, No. 3, 2007, pp. 439-44.
- Sarici, Dilek, et al. "Thyroid functions of neonates with Down syndrome." Italian Journal of Paediatrics, Vol. 38, No. 1, 2012, p. 44.
- Shriraam, M., and M. Sridhar. "Subclinical hypothyroidism in children." Indian Paediatrics, Vol. 51, No. 11, 2014, pp. 889-895.
- Dayal, Devi, et al. "Thyroid dysfunction in Indian children with Down syndrome." Indian Pediatrics, Vol. 51, No. 9, 2014, pp. 751-53.
- Zwaveling-Soonawala, Nitash, et al. "Early thyroxine treatment in Down syndrome and thyroid function later in life." European Journal of Endocrinology, Vol. 176, No. 5, 2017, pp. 505-13.
- Lavigne, Jenifer, et al. "Thyroid dysfunction in patients with Down syndrome: Results from a multi‐institutional registry study." American Journal of Medical Genetics Part A, Vol. 173, No. 6, 2017, pp. 1539-45.
- Purdy, I. B., et al. "Revisiting early hypothyroidism screening in infants with Down syndrome." Journal of Perinatology, Vol. 34, No. 12, 2014, pp. 936-40.
- Hardy, Olga, et al. "Hypothyroidism in Down syndrome: Screening guidelines and testing methodology." American Journal of Medical Genetics Part A, Vol. 124, No. 4, 2004, pp. 436-37.
- Mattheis, P. "Thyroid disease in Down’s syndrome: clinical perspective, directions of research." 2nd International Symposium on Biomedical and Psychoeducational Aspects on Down Syndrome, Mexico City, 1997.
- Moosa, Shahida, et al. "Thyroid dysfunction in a cohort of South African children with Down syndrome." South African Medical Journal, Vol. 103, No. 12, 2013, pp. 966-70.